 By Rushad Dordi, MD
By Rushad Dordi, MD
Peer Reviewed
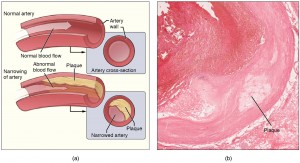
This week’s Primecuts details four examples of novel methodologies for treating common diseases. We begin first with a study repurposing an anti-inflammatory therapeutic for the treatment of atherosclerosis, …

 By Rushad Dordi, MD
By Rushad Dordi, MD
Peer Reviewed
This week’s Primecuts details four examples of novel methodologies for treating common diseases. We begin first with a study repurposing an anti-inflammatory therapeutic for the treatment of atherosclerosis, …
 By Scarlett Murphy, MD
By Scarlett Murphy, MD
Peer Reviewed
American attention shifted away from challenging national conversations in the wake of Charlottesville towards the sky this past Monday, when a total solar eclipse traversed …
 By Andrew Armanious, MD
By Andrew Armanious, MD
Peer Reviewed
This past week, President Trump decided to part ways with White House Chief Strategist Steve Bannon (1). Bannon was a controversial and blunt-spoken political figure who influenced President …
 By Jonathan Whitehouse, MD
By Jonathan Whitehouse, MD
Peer Reviewed
In New York last week, Mayor de Blasio announced a plan to tax wealthy New Yorkers in order to raise funds for our enfeebled subway system. …
 By Christopher Sonne, MD
By Christopher Sonne, MD
Peer Reviewed
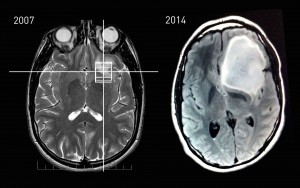
It is the last admission of your admitting night shift. You are called to assess a pleasant, oriented 65-year-old man with lung cancer and …
 By Jiwoon Chang, MD
By Jiwoon Chang, MD
Peer Reviewed
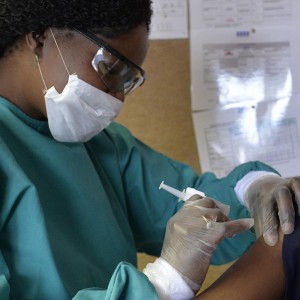
This past week at the International AIDS Society Conference in Paris, investigators of the mosaic HIV vaccination trial called APPROACH shared …
 Kelsey Luoma, MD
Kelsey Luoma, MD
Peer Reviewed
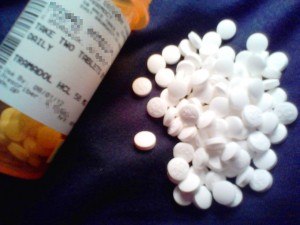
Opioid-related morbidity and mortality has reached crisis levels in the United States. According to the CDC, between 1999 and 2014 more than 165,000 people died due to …
By Cesar Soria Jimenez, MD
Peer Reviewed
 In this week’s Primecuts issue, we will be discussing topics related to obesity and its effects on the global population over the past quarter century …
In this week’s Primecuts issue, we will be discussing topics related to obesity and its effects on the global population over the past quarter century …