 Nicholas Mark, MD & Sarah Buckley, MD
Nicholas Mark, MD & Sarah Buckley, MD
Faculty Peer Reviewed
Background
Publius Aelius Hadrianus, better known as Hadrian, emperor of Rome (117-138 CE), traveler, warrior, and lover of all things Greek, fell ill at the age of 60. He developed progressive edema and episodic epistaxis, …

 By Michael Boffa
By Michael Boffa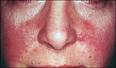
 By Ivan Saraiva, MD
By Ivan Saraiva, MD  By Joshua Farhadian
By Joshua Farhadian By Benjamin Kenigsberg
By Benjamin Kenigsberg By Santosh Vardhana
By Santosh Vardhana By Santosh Vardhana
By Santosh Vardhana