Introduction to Cases:
During the upcoming weeks, we will post a series of cases addressing the appropriate treatment for patients with stable coronary artery disease. We will be focus on indications for revascularization in stable angina. In all of the cases, the patients will be at high enough risk that stress tests and coronary angiography will be performed.
There has been recent data and recommendations on the appropriate indications for revascularization in stable angina. These recommendations are based on clinical symptoms, non-invasive imaging, and catheterization findings. After reading through these cases, we hope you have a better understanding of what the appropriate indications are for revascularization, and the evidence behind them.
Ramin Shayegan Hastings MD, Jonathan Willner MD, and Steven Sedlis MD
Case #2:
A 59-year-old male with hypertension and hyperlipidemia comes into your clinic for evaluation of chest pain. The patient states that for the past few months he has been having chest pain on exertion. He describes a substernal chest pain that radiates to the L arm after walking about 10 blocks or climbing 2 flights of stairs. The pain is relieved with approximately 5 minutes of rest. He denies any other associated symptoms, and has never had the pain at rest. He has had hypertension for the past 15 years, currently being treated with hydrochlorothiazide 25 mg daily and lisinopril 10 mg daily. His resting BP is 136/88. He also takes simvastatin 40 mg daily for an elevated LDL, which is now 110.
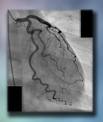
Electrocardiogram (ECG) done in the office reveals normal sinus rhythm with HR of 72 and non-specific ST segment and T wave changes in the anterior-lateral leads. He is referred for an exercise stress test with nuclear imaging. His exercise stress was notable for 3 mm ST depressions in the anterior leads after 10 minutes of exercising. He had to stop the test secondary to chest pain after the 10 minutes. The nuclear portion of the stress test showed a large reversible perfusion defect affecting the anterior wall of the left ventricle, with an ejection fraction of 45%. Subsequent cardiac catheterization reveals a 75% stenosis of the proximal left anterior descending (LAD) artery, along with 80% stenosis of the mid left circumflex artery.
What is the appropriate next step in management of this patient?
A. No further treatment necessary
B. Medical therapy alone, including anti-anginal medication, aggressive blood pressure control, lipid reduction, smoking cessation, and an exercise program.
C. Cardiac viability study followed by revascularization if tissue is viable, along with medical therapy
D. Revascularization of the lesions with either percutaneous coronary intervention (PCI) or coronary artery bypass grafting (CABG) along with medical therapy
Answer: D
This patient is a hypertensive male with hyperlipidemia presenting with symptoms consistent with angina pectoris. He has CCS class II symptoms (see previous post) (1). His stress tests have high-risk features (2) (see previous post–Duke treadmill score of -13 and large area of reversible ischemia on imaging). His coronary angiogram shows severe stenoses of the proximal LAD and mid circumflex arteries. This patient is certainly at higher risk for subsequent cardiac events and cardiac death than the patient presented in Case #1 (see previous post).
Older studies, including three large randomized trials comparing revascularization (CABG) to medical therapy included patients like this with high-risk features (Veterans Affairs Cooperative Study (4), European Coronary Surgery Study (5), and Coronary Artery Surgery Study (CASS (6)). A meta-analysis of these studies found a survival benefit with revascularization only in patients with three vessel, left main, or proximal LAD lesions (7). Based largely on this data, the American College of Cardiology and American Heart Association recommend revascularization for patients with left main disease, three vessel disease, or two-vessel disease involving the proximal LAD (along with abnormal LV function, or ischemia on non-invasive testing) as class IA recommendations. They recommend PCI for non-diabetic patients with 1 or 2 vessel disease involving the proximal LAD and normal LV function (class IB recommendation). PCI is also recommended for any patient with high-risk findings on non-invasive imaging (class IB) (8).
However recent data, including the COURAGE trial (3), have shown that medical therapy is as efficacious as revascularization in many settings of stable angina (see previous post). Patients with proximal LAD lesions were included in the COURAGE trial (34% of subjects had proximal LAD lesions), and only patients with very high-risk features on non-invasive testing were excluded (blood pressure drop or extensive ST depression during the first 3 minutes of the Bruce protocol). In addition, patients with disabling angina (CCS class IV), left ventricular ejection fraction less than 30%, or left main disease were excluded. The major difference between COURAGE and previous studies of revascularization in stable angina was the inclusion of aggressive medical therapy in the control group. Patients randomized to medical therapy in COURAGE received anti-platelet therapy (aspirin or plavix), long-acting metoprolol, amlodipine, isosorbide mononitrate (in combination or alone), along with either linisopril or losartan. All patients received aggressive lipid lowering therapy (target LDL of 60-85, HDL > 40, and triglycerides < 150). Previous studies mentioned above did not provide this level of medical therapy to the control group. Given these disparate findings, a new study is currently in the planning stages which will randomize high risk patients to aggressive medical therapy and revascularization versus aggressive medical therapy alone (International Study of Comparative Health Effectiveness with Medical and Invasive Approaches – ISCHEMIA). This study may provide more insights on the appropriate treatment for this patient.
Based on the currently available data, the appropriateness guidelines for revascularization in stable angina (see previous post (9)) state that any patient with high-risk findings on noninvasive imaging has an appropriate indication for revascularization (only exception is an uncertain rating for 1-2 vessel disease without proximal LAD disease in asymptomatic patients, and total occlusion of 1 vessel in asymptomatic or class I/II angina off medication). In patients with 2-vessel disease involving the proximal LAD, revascularization is appropriate when symptoms are present (except with low-risk findings on non-invasive testing and CCS class I/II symptoms off medication). Based on recommendations from the AHA/ACC and the appropriateness guidelines, revascularization is appropriate in this patient with high-risk findings on non-invasive imaging and high risk coronary artery lesions (Answer Choice D). However, the current literature is unclear whether this approach will have any effect on cardiac morbidity and mortality. This is clearly an area for future research.
References
1. Campeau L. The Canadian Cardiovascular Society grading of angina pectoris revisited 30 years later. Can J Cardiol2002 Apr;18(4):371-9. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=11992130
2. Gibbons RJ, Balady GJ, Bricker JT, Chaitman BR, Fletcher GF, Froelicher VF, Mark DB, McCallister BD, Mooss AN, O’Reilly MG, Winters WL, Jr., Antman EM, Alpert JS, Faxon DP, Fuster V, Gregoratos G, Hiratzka LF, Jacobs AK, Russell RO, Smith SC, Jr. ACC/AHA 2002 guideline update for exercise testing: summary article: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1997 Exercise Testing Guidelines). Circulation2002 Oct 1;106(14):1883-92. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=12356646
3. Boden WE, O’Rourke RA, Teo KK, Hartigan PM, Maron DJ, Kostuk WJ, Knudtson M, Dada M, Casperson P, Harris CL, Chaitman BR, Shaw L, Gosselin G, Nawaz S, Title LM, Gau G, Blaustein AS, Booth DC, Bates ER, Spertus JA, Berman DS, Mancini GB, Weintraub WS. Optimal medical therapy with or without PCI for stable coronary disease. N Engl J Med2007 Apr 12;356(15):1503-16. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=17387127
4. Eighteen-year follow-up in the Veterans Affairs Cooperative Study of Coronary Artery Bypass Surgery for stable angina. The VA Coronary Artery Bypass Surgery Cooperative Study Group. Circulation1992 Jul;86(1):121-30. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=1617765
5. Varnauskas E. Twelve-year follow-up of survival in the randomized European Coronary Surgery Study. N Engl J Med1988 Aug 11;319(6):332-7. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=3260659
6. Coronary artery surgery study (CASS): a randomized trial of coronary artery bypass surgery. Survival data. Circulation1983 Nov;68(5):939-50. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=6137292
7. Yusuf S, Zucker D, Peduzzi P, Fisher LD, Takaro T, Kennedy JW, Davis K, Killip T, Passamani E, Norris R, et al. Effect of coronary artery bypass graft surgery on survival: overview of 10-year results from randomised trials by the Coronary Artery Bypass Graft Surgery Trialists Collaboration. Lancet1994 Aug 27;344(8922):563-70. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=7914958
8. Gibbons RJ, Chatterjee K, Daley J, Douglas JS, Fihn SD, Gardin JM, Grunwald MA, Levy D, Lytle BW, O’Rourke RA, Schafer WP, Williams SV. ACC/AHA/ACP-ASIM guidelines for the management of patients with chronic stable angina: executive summary and recommendations. A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Management of Patients with Chronic Stable Angina). Circulation1999 Jun 1;99(21):2829-48. http://circ.ahajournals.org/cgi/content/full/99/21/2829
http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=10351980
9. Patel MR, Dehmer GJ, Hirshfeld JW, Smith PK, Spertus JA. ACCF/SCAI/STS/AATS/AHA/ASNC 2009 Appropriateness Criteria for Coronary Revascularization: A Report of the American College of Cardiology Foundation Appropriateness Criteria Task Force, Society for Cardiovascular Angiography and Interventions, Society of Thoracic Surgeons, American Association for Thoracic Surgery, American Heart Association, and the American Society of Nuclear Cardiology: Endorsed by the American Society of Echocardiography, the Heart Failure Society of America, and the Society of Cardiovascular Computed Tomography. Circulation2009 Mar 10;119(9):1330-52. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=19131581

2 comments on “Appropriateness for Revascularization in Stable Angina”
Comments are closed.