 Commentary by Peter Izmirly MD, NYU Division of Rheumatology
Commentary by Peter Izmirly MD, NYU Division of Rheumatology
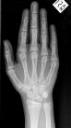
A 54 year old male with a past medical history significant for hepatitis C genotype 1a s/p ifn/ribavarin 2003-2004 with HCV Qual negative in 2005 presents with 3 weeks of bilateral wrist pain. The pain is worst with extension. His exam is notable for diffuse tenderness when pressure is applied to his wrists. He has no obvious swelling, erythema, deformity or subcutaneous nodules. The remainder of his musculoskeletal exam in unremarkable. In addition, he has no stigmata of cirrhosis. Labs were sent, revealing normal CBC, normal LFTS, including an albumin of 5.1 and an INR of 1.1. His ESR was <20 and his CRP was normal. RF was 213 with normal being (0-39). X-rays of hands and wrist were unremarkable other than mild osteoarthritis of 1st MCP bilaterally.
When a patient presents with polyarticular joint pain, a thorough history and physical exam is essential.
Keys include:
Number of joints involved
Symmetry
Presence of morning stiffness
Is pain worse with movement
Insidious or acute
Joint swelling/erythema
Rheumatologic ROS (alopecia, oral ulcers, rashes-psoriasis, eye erythema and pain, oral ulcers, Raynaud’s, parasthesias, etc)
Recent viral illness, bloody diarrhea, STDs, hepatitis
Medication history, including diuretics
In this case, you know the patient has a history of treated hepatitis C. In addition, you have the luxury of having x-rays that reveal no signs of an inflammatory arthritis (osteopenia, joint space narrowing or erosions) and acute phase reactants that are normal, which are both reassuring. A positive rheumatoid factor in this setting, even though it is high titer, does not indicate the patient has rheumatoid arthritis. Although an elevated rheumatoid factor could be a mark of RA, and although this patient has symmetrical wrist involvement such as might be seen in RA, he also has two reasons that are more likely to explain his elevated rheumatoid factor. Hepatitis C has been associated with elevated rheumatoid factor, and hepatitis C has also been associated with mixed cryoglobulinemia (types II and III) which by definition means having a positive rheumatoid factor.
Depending on the cohort studied, arthritis is present in up to 20 percent of HCV patients. In two thirds of the cases, the arthritis mimics a rheumatoid arthritis (i.e., symmetrical, including hand/finger involvement) type picture with the remaining third having a waxing a waning oligoarthritis type picture (1). Most likely, the arthritis in this setting is due to immune complex formation between the hepatitic C virus and anti-hep C antibodies. Accordingly, the arthritis may occur when the antigen/antibody reach a particular ratio leading to immune complex formation, and this may occur early, late or chronically. The treatment of choice for this type of arthritis is nonsteroidal anti-inflammatory drugs (NSAIDs) with close monitoring of liver function and possibly the use of hydroxychloroquine. Because the arthritis is typically mild, treatment of the hepatitis C with antivirals in this setting is generally deferred to the hepatologist, who will make their decision based on the need to address the liver infection itself.
This patient may also have mixed cryoglobulinemia. Cryoglobulinemia associated arthritis consists of an intermittent, mono or oligoarticular, nondestructive arthritis affecting large and medium size joints and is caused by deposition of circulating immune complexes depositing in the joints. However, these circulating immune complexes will typically consist of an anti-hepatitis C antibody and the rheumatoid factor, which is simply antibody directed at immunoglobulins. In many cases, cryoglobulinemic arthritis is accompanied by other symptoms of cryoglobulinemia (ex, nephritis, vasculitis, including skin, bowel and CNS), and since these can be severe, treatment usually consists of treating the underlying Hepatitis C infection. Although this is frequently helpful, cyroglobulins can sometimes persist even after Hep C has been eradicated. Recently, rheumatologists and nephrologists have begun to employ rituximab, an anti-B cell antibody, to lower cryoglobulins with good effect. As this strategy is relatively new, not fully tested and has some possible serious adverse effects, it should be left to physicians with experience in rituximab use.
In this patient, I would favor the diagnosis of arthritis associated with cryoglobulinemia over arthritis associated with Hep C per se, as the patient has been treated for hepatitis C, has a negative viral load but a persistently positive rheumatoid factor. His lack of cutaneous signs of cryoglobulinemia such as palpable purpura or livedo reticularis argues against this diagnosis. However. I would check for cryoglobulins and hepatitis C viral load if neither has been recently checked. Since he does not have stigmata of serious cyroglobulinemia, he can be managed symptomatically with an NSAID in any event. The patient does not currently meet criteria for RA as he does not meet four out of the seven ACR criteria (symmetric polyarthritis; arthritis of three or more joints; MCP, PIP or wrist involvement; morning stiffness greater than or equal to one hour, positive rheumatoid factor, marginal erosions on X-ray, duration of symptoms greater than six weeks, and rheumatoid nodules.) However, I would order an anti-CCP antibody level since anti-CCP antibodies are more specific for RA than is RF. A positive anti-CCP antibody would compel at least a reconsideration of the possibility of RA. As in many rheumatic diseases, patience is key and his disease may take time to evolve. It’s important to maintain an open mind about the possibility that the initial diagnosis is not correct. I would continue to follow him on a routine basis, every 4 months, to see how the patient is doing and to see if any other symptoms develop which could change my thinking about the case.
1. Rosner, I, Rozenbaum, M, Toubi, E, et al. The case for hepatitis C arthritis.
Semin Arthritis Rheum 2004; 33:375.

One comment on “How Do You Approach a Patient with Arthritis and Hepatitis C?”
Wonderfully related and intelligently explained.
Important publication for patients as well as physicians.
Comments are closed.