 Commentary by Rosemary Adamson MD, PGY-2
Commentary by Rosemary Adamson MD, PGY-2
Be on the look-out for measles! New York City’s Department of Health and Mental Hygiene (DOHMH) issued a measles alert at the end of last November because there were 5 confirmed cases of measles being imported from abroad in 2007 to NYC. The DOHMH wished to raise healthcare provider awareness of measles, especially in travelers. Coming from the UK, this alert is close to my heart, as Britain has been battling with reduced uptake of the MMR vaccine and consequent increased numbers of measles cases for several years. Indeed, one of the imported measles cases came from the UK; the others were from Belgium, China, Israel and Japan. Two of the five cases were US residents and three were foreign nationals. They were a mix of adults and children. However, once measles is imported it becomes a local problem – in 2006 at least 14 cases of measles in Boston were thought to have been caused by spread from a traveler from India. Canada had an annual national average of 10 cases per year from 2002 to 2006 but this year there have been nearly 100 cases of measles in Quebec alone, illustrating the infectivity of this virus.
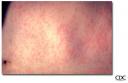
Measles is an acute viral illness caused by an RNA paramyxovirus. It is highly contagious, infecting non-immune individuals i.e. those who have been neither exposed nor fully immunized. It is important to note that one vaccination is insufficient to develop full immunity. In epidemics, attack rates of 99% have been recorded. The incubation period lasts 6-14 days and individuals become contagious as soon as they develop any symptoms through until a few days after the rash appears. The first symptoms consist of a prodrome of cough, coryza and conjunctivitis (“the 3 Csâ€) with fever up to 105ºF. Two or three days later the main illness develops with its characteristic rash and Koplik spots. The rash is maculopapular and erythematous, starting on the face and the working down the body and on to the limbs, including the palms and soles. It may become confluent over the trunk. Koplik spots are small white spots on the mucous membranes of the oropharynx, especially the buccal mucosa, and are pathognomonic, but not always visible. Most cases are relatively benign and resolve spontaneously. Management is entirely supportive as there is no specific treatment for this disease.
Case fatality is due to complications which range from mild to severe and tend to be worse in older patients. They include diarrhea and respiratory tract infections such as bronchitis and otitis media, both of which may require antibiotics, if there appears to be secondary bacterial infection. Another complication is giant cell pneumonia due to direct invasion of the lungs by the measles virus, which is rare, occurring in immunocompromised individuals. Devastating neurological sequelae also may occur. Post-infectious encephalitis occurs in approximately one in every thousand cases. It develops within a few days of the rash and commonly presents with drowsiness, headache and convulsions. Mortality approaches 50% and survivors typically are left with neurological deficits. Subacute Sclerosing Panencephalitis (SSPE) is a fatal condition which can occur many years after measles, more commonly in those who acquired measles under 1 year of age. The New England Journal of Medicine recently published a case report of this complication.
Measles is a reportable disease – any suspected cases must be placed in respiratory isolation, the NYC DOHMH Bureau of Immunization must be immediately notified (weekdays call 212-676-2284 and after hours call 212-764-7667) and a thorough travel history should be obtained from the patient and their immediate contacts. Contacts should be vaccinated within 72 hours of exposure. Any contacts who have previously received vaccination should receive a booster. Immune globulin should be administered to non-immune contacts, especially if they are pregnant women and children less than 1 year old, and any immunocompromised contacts, regardless of prior vaccination.
Diagnosis should be confirmed by serologic testing of blood samples for IgM. IgM may be negative in the first 72 hours after onset of rash and should therefore be repeated after a couple days if negative in a patient who has had a characteristic rash for less then 72 hours. IgM will persist for approximately one month from the onset of the rash. Specimens from all suspected cases should be delivered to the Public Health Laboratory just down the road at 455 1st Ave (call 212-447-6112 with any questions about specimens). Blood samples should be drawn into red-topped vacutainer tubes. If necessary the DOHMH can arrange virus isolation from urine, nasopharyngeal or throat swab specimens.
The DOHMH issued its warning at the end of November because the holiday season is a time of increased travel. So please look out for the measles prodrome among all the URIs you will see this winter and remember that measles is highly contagious and potentially fatal.
To sign-up to receive free email health alerts from the NYC Department of Health and Mental Hygiene visit:
http://www.nyc.gov/html/doh/html/hcp/hcp.shtml#han
References:
NYC DOHMH 2007 Alert #35: Measles Among International Travelers. http://www.nyc.gov/html/doh/downloads/pdf/cd/07md35.pdf Accessed December 24, 2007
Public Health Agency of Canada. Information for Health Professionals: Measles.
http://www.phac-aspc.gc.ca/im/meas-roug/index_e.html#os Accessed December 24, 2007
http://en.wikipedia.org/wiki/Measles
Timothy, McCartney, Thacker & Ward Notes on Medical Microbiology. 1st Ed. Churchill Livingstone 2002:365-368
Strohl, Rouse & Fisher Lippincott’s Illustrated Reviews: Microbiology. 1st Ed. Lippincott Williams & Wilkins 2001:383-384
Image courtesy of CDC
