 Chief complaint: 85 year old female presents with worsening shortness of breath for one day.
Chief complaint: 85 year old female presents with worsening shortness of breath for one day.
History of present illness:
The patient’s history of present illness begins at the age of 60 when she was diagnosed with asthma, for which she had been treated with inhaled anticholinergics, beta agonists and intermittent oral steroids. Twelve years prior to admission, the patient was diagnosed with diabetes, which was managed with oral medications. Two years prior to admission, the patient was diagnosed with Mycobacterium avium complex (MAC) at an outside hospital and received a full course of treatment. On the day prior to admission, the patient noted a worsening cough productive of green sputum, along with wheezing and shortness of breath. The patient was evaluated by her primary doctor and started on prednisone 20 mg twice a day. However, after two doses of prednisone, she reported feeling worse and was instructed by her doctor to come to the ER.
Physical exam was significant for a lung exam with diffuse wheezes, but with adequate air movement.
Chest X-ray: bronchiectasis; no effusions, consolidation, or infiltrates
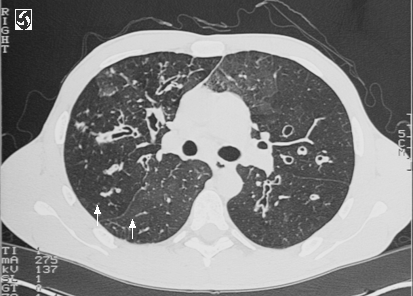
The patient was initially treated with solumedrol 125 mg IV along with atrovent/albuterol nebulizers. The following morning, a sputum culture was obtained and the patient was started on azithromycin. Over the course of the next four days, steroids, azithromycin, and nebulizers were continued with little improvement. Sputum culture revealed normal flora. On hospital day number 5, a chest CT was performed, revealing bronchiectasis and evidence of extensive of prior granulomatous disease with diffuse lymphadenopathy and calcified granulomata. A repeat sputum culture grew pseudomonas, and the patient was subsequently started on Cefepime, which was changed to ciprofloxacin after the patient developed a rash. On ciprofloxacin, the patient gradually improved over the next five days to her baseline. She was discharged on a prednisone taper, with plans to complete a ten day course of ciprofloxacin.
Teaching points:
1. Bronchiectasis is an inflammatory reaction resulting in the dilation of airways with thickened walls. It can be secondary to COPD or can be independent of COPD in a patient with an infectious insult in the setting of airway blockage or an immunocompromised state.
2. Clinically, bronchiectasis can look very similar to COPD, with sputum production, cough, frequent pulmonary infections, dyspnea, and hemoptysis. Diagnosis is by CT scan, with evidence of dilated airways, frequently with fluid pooling.
3. Treatment for bronchiectasis differs from treatment for COPD. Bronchiectatic airways with or without additional COPD are very susceptible to colonization/infection with multiple organisms, including pseudomonas, MAI, H. flu, and aspergillus. Antibiotic therapy should be directed toward such organisms. It is frequently difficult to differentiate between acute infection with these organisms and colonization. Colonization with pseudomonas is associated with more extensive bronchiectasis on CT and more frequent hospitalizations.
