Before you read the answer, you may want to review the initial Mystery Quiz posted last week.
Commentary by Andrew Hardie MD, Fellow, NYU Department of Radiology
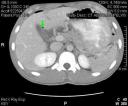
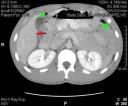
Although this patient’s symptoms were not the most typical of this entity, the CT findings in this case are diagnostic of a perforated anterior duodenal ulcer. The most essential observation, and the one that alters management, is the presence of intraabdominal free air (arrows). The small collections of air in this case are not unusual for bowel perforations, especially proximally. One can see how occasionally these small volumes of free air may not be able to be seen on plain films, especially inadequately positioned films.
The specific location of the free air in this case directs one to suspect a duodenal perforation. Air is seen in the periportal region, around the duodenum (green arrows), and in this case, at the site of the perforation in the duodenal wall (red arrow).
A point of interest is that only the anterior duodenal bulb wall is intraperitoneal. Therefore, this must be an anterior wall ulcer. A posterior wall ulcer will lead to gastrointestinal bleeding, because, if you remember your anatomy, the gastroduodenal artery lies directly posterior to the duodenal bulb. Although very rare, a perforated posterior wall ulcer would cause retroperitoneal air, not intraperitoneal air.
The patient in this case reported severe epigastric pain, which could be indicative of peptic ulcer disease. However, physical exam was not suggestive of peritonitis. It is important to remember that atypical presentations of perforated ulcers can occur, although this is more commonly seen in elderly patients. Also, in this case, the perforation could have occurred in the interval between admission and abdominal imaging. The patient was taken to the OR for immediate repair of the perforation and postoperative clinical course was uneventful. Upon further questioning, he did admit to heavy weekend alcohol use as well as recent increased NSAID use for some low back pain.