Posted By: Vivian Hayashi, MD, Instructor of Clinical Medicine, Division of General Internal Medicine and Robert Smith, MD Associate Professor of Medicine, Division Pulmonary and Critical Care Medicine
A 78 year old man with a history of ankylosing spondylitis and known cardiac disease associated with congestive heart failure, presented with breathlessness one year prior to admission. Over the most recent months, the patient complained of cough productive of voluminous frothy, watery sputum. Medications included digoxin, furosemide, irbesartan, isosorbide, metoprolol, spirinolactone, simvastatin, and warfarin. The patient had worked as a photographer, mixing his own chemicals. He was an ex-smoker who quit 45 years earlier.
Prone imaging showed no changes in the location of the abnormalities
Several months later, the patient reported worsening symptoms. Repeat imaging showed the following:
Transbronchial biopsy did not reveal infection nor malignancy and PAS staining was negative. Â An open biopsy was performed.

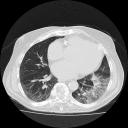
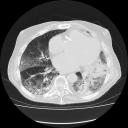
One comment on “Mystery Quiz”
Comments are closed.