Faculty peer reviewed by Rardi Feigenbaum MD
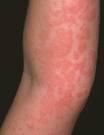
Urticaria is a common cutaneous disorder characterized by transient edematous plaques resulting from acute dermal edema and surrounding erythema. Roughly 20% of the general population will manifest urticaria at some point in their lives, qualifying it as a condition caregivers should be able to recognize and treat. When the unsightly wheal and flare reaction combined with periods of intense pruritis persists for greater than six weeks without an identifiable causative agent, the condition is referred to as chronic idiopathic urticaria (CIU).
While the majority of CU is categorized as idiopathic, in roughly one third to one half of patients autoimmunity appears to drive the disease process. Of patients with autoimmune chronic urticaria, more than half have functional autoantibodies against the high-affinity IgE receptor FcεR1 located on skin mast cells. Another 10% are found to have circulating anti-IgE IgG. A significant fraction of patients with autoimmune urticaria also have antithyroglobulin and/or antimicrosomal antibody, with or without abnormal thyroid function.
Although controversial, some authors suggest that the etiology of disease for a portion of CIU patients is a pseudoallergy to food ingredients. The concept of pseudoallergic reactions was introduced in 1983 to describe responses to a food or chemical that mimicked the signs and symptoms of an allergic reaction but without isolation of specific IgE antibodies against the offending agent. Implicated agents include preservatives, sweeteners, artificial food dyes, aromatic volatile compounds in tomatoes, herbs, wine, salicylic acid, orange oil, alcohol, high dietary fat. Various studies report remission rates due to elimination diets ranging between 31% and 100%, including ‘full’ and ‘partial’ responders, however, as a long-term treatment plan these strict diets are often difficult to adhere to. Elimination diets can occasionally be useful in diagnosis (i.e. symptoms resolve when a particular food is avoided and reoccur when the food is reintroduced), but more often than not a causative agent is not identified. A pilot study published this fall in Clinical and Experimental Allergy outlines a stepwise reintroduction diet for patient’s who have demonstrated complete remission during an elimination diet as a means to identifying individual problem foods.
Chronic urticaria can be frustrating to treat as some patients may not improve or may require years of medication for symptom control. Though often overlooked as a trivial condition, the physical, functional and psychosocial consequences of chronic urticaria can be debilitating. In fact, one study found that the degree of disability and lowered quality of life experienced by those with CIU rivals that of older patients with ischemic heart disease. Not only does CIU negatively impact health and quality of life but it also imparts a significant financial burden on individuals as well as society. In addition to direct costs of medication, one study calculated 25 to 30% lost productivity at work, school, or in daily activities among CIU sufferers.
The newer second generation H1 antihistamines are replacing their older counterparts as first-line therapy for symptomatic urticaria. These agents are either non-sedating or at least less sedating than first generation H1 blockers with an overall favorable safety profile. Included in this group are loratadine, desloratadine, fexofenadine, and cetirizine.
Levocetirizine is among the newest in this class and after several years on the European market was approved in May 2007 for use in the United States in the treatment of symptoms associated with seasonal perennial allergic rhinitis and for uncomplicated skin manifestations of CIU. The clinical efficacy of levocetirizine for the treatment of CIU in adults has been established in three large multicenter, well controlled trials, though notably these are trials of drug vs. placebo.
The use of antihistamines in CIU makes sense because histamine is largely responsible for the urticarial triad of wheals, erythema, and pruritis. Interestingly, however, disease activity has been linked to a variety of other pro-inflammatory molecules and an increasing body of evidence suggests that newer antihistamine agents also modulate these disease-driving processes. Increased levels of cellular adhesion molecules (CAMs) have been demonstrated in physical and chronic idiopathic urticarias suggesting a role for these transmembrane protein receptors in disease pathogenesis. CAMs are thought to control recruitment, migration, and activation of inflammatory cells in sites of inflammation. In a recent study, CAM levels (specifically ELAM-1 and P-selectin) decreased with use of a second generation antihistamine, paralleling clinical improvement in patients with chronic urticaria. Second generation antihistamines have also demonstrated efficacy in inhibiting cytokine release from mast cells and basophils in vitro, suggesting another anti-inflammatory mechanism of action for this drug class.
Some patients will exhibit intolerance or resistance to antihistamines and alternative therapies are available including leukotriene modifiers, dapsone, sulfasalazine, or hydroxychloroquine. Evidence supporting efficacy of most of these treatments, however, is currently limited to anecdotal accounts. In refractory cases it would be prudent to refer patients to an allergist or dermatologist before initiating second-line therapy.
With the addition of a safe and effective new pharmaceutical, the discovery of other disease-driving mechanisms and thus new targets for therapy, and the development of a method for identifying urticaria-inducing food which takes into account personal tastes and eating habits, urticaria-sufferers have cause to stop scratching and smiling again.
Commentary by Rardi Feigenbaum, MD, Clinical Assistant Professor, NYU Department of Medicine
This post brings up some important points regarding urticaria:
–Urticaria (with or without angioedema) is common. It is one of the most common diagnoses seen by allergists.
–Urticaria can be a very frustrating condition for the patient. Its seemingly random onset and waxing and waning nature and overlap of symptoms with many allergic (IgE mediated) syndromes convinces most patients there is a hidden allergen which is causing the condition. However, over the years, studies have consistently refuted this theory and a “cause” is rarely in Chronic Idiopathic Urticaria (CIU.)
–I think that most allergists would consider the “pseudoallergy” food theory of urticaria to be very, very controversial, although “never say never…”
–Most patients can be controlled with the right combination of meds.
References
1. Adelsberg BR. Sedation and performance issues in the treatment of allergic conditions. Arch Intern Med. 1997; 157:494-500.
2. Gaillard AW, Gruisen A, de Jong R. The influence of antihistamines on human performance. Eur J Clin Pharmacol. 1988;35:249-253.
 3. Grant JA, Riethuisen JM, Moulaert B, DeVos C. A double-blind, randomized, single-dose, crossover comparison of levocetirizine with ebastine, fexofenadine, loratadine, mizolastine, and placebo: suppression of histamine-induced wheal-and-flare response during 24 hours in healthy male subjects. Ann Allergy Asthma Immunol. 2002;88:190-197.
4. Kay GG, Quig ME. Impact of sedating antihistamines on safety and productivity. Allergy Asthma Proc. 2001;22:281-283.
5. KÅ‚os K, Kruszewski J, Kruszewski R, SuÅ‚ek K. The effect of 5-days of cetirizine, desloratadine, fexofenadine 120 and 180 mg, levocetirizine, loratadine treatment on the histamine-induced skin reaction and skin blood flow–a randomized, double-blind, placebo controlled trial. Pol Merkur Lekarski. 2006;21:449-453.
6. Molimard M, Diquet B, Benedetti MS. Comparison of pharmacokinetics and metabolism of desloratadine, fexofenadine, levocetirizine and mizolastine in humans. Fundam Clin Pharmacol. 2004;18:399-411.
7. O’Donnell BF, Lawlor F, Simpson J, Morgan M, Greaves MW. The impact of chronic urticaria on quality of life. Br J Dermatol. 1997;136:197-201.
8. Tong LJ, Balakrishnan G, Kochan JP, Kinét JP, Kaplan AP. Assessment of autoimmunity in patients with chronic urticaria. J Allergy Clin Immunol. Apr 1997;99(4):461-5.
9. Witek TJ Jr, Canestrari DA, Miller RD, Yang JY, Riker DK.  Characterization of daytime sleepiness and psychomotor performance following H1 receptor antagonists. Ann Allergy Asthma Immunol. 1995;74:419-426.
Â
Â