During the upcoming weeks, we will post a series of cases addressing the appropriate treatment for patients with stable coronary artery disease. We will be focus on indications for revascularization in stable angina. In all of the cases, the patients will be at high enough risk that stress tests and coronary angiography will be performed.
There has been recent data and recommendations on the appropriate indications for revascularization in stable angina. These recommendations are based on clinical symptoms, non-invasive imaging, and catheterization findings. After reading through these cases, we hope you have a better understanding of what the appropriate indications are for revascularization, and the evidence behind them.
Ramin Shayegan Hastings MD, Jonathan Willner MD, and Steven Sedlis MD
Case 1:
A 54-year-old male with a past medical history of hypertension (well-controlled on hydrochlorothiazide 25 mg daily) and tobacco use (20 pack-year) presents for evaluation of chest pain. The patient states that for the past 3 months he has noted chest pain on exertion. During normal walking he does not have chest pain, however whenever he runs or walks fast for more than a couple of minutes, he experiences chest pain. The pain is substernal, non-radiating, and associated with mild shortness of breath and slight diaphoresis. He also notes chest pain after climbing 2-3 flights of stairs.
Patient denies any chest pain at rest, paroxysmal nocturnal dyspnea, orthopnea, or lower-extremity edema. He has a family history of coronary artery disease in his father who had a myocardial infarction (MI) at the age of 40. He takes no other medications except for hydrochlorothiazide 25 mg daily.
Physical exam is largely unremarkable with BP 126/62 and HR 82. Electrocardiogram (ECG) done in the office reveals normal sinus rhythm with slight ST depressions and t-wave flattening in the lateral leads.
He is then referred for an exercise stress test. After 15 minutes on the Bruce Protocol he develops 2 mm ST depressions in leads V2-V4, with no associated chest pain. His nuclear stress test reveals a small reversible perfusion defect in the lateral left ventricular wall. His EF is noted to be 50%. Cardiac catheterization reveals a focal 85% stenosis in the second obtuse marginal branch of the proximal Left Circumflex Artery along with a focal 70% stenosis of his distal Right Coronary Artery.
Which of the following is the best treatment approach?
A. No treatment is necessary
B. Medical therapy alone, including anti-anginal medication, aggressive blood pressure control, lipid reduction, smoking cessation, and an exercise program
C. Revascularization of the Obtuse Marginal branch of the Left Circumflex Artery
D. Revascularization of the Right Coronary Artery
E. Revascularization of both the Obtuse Marginal branch of the Left Circumflex and Right Coronary Arteries
Answer: B
In this case, we have a male with risk factors for coronary artery disease including hypertension, smoking, and family history of early heart disease. He is presenting with symptoms concerning for angina.
Typical (definite) angina is defined as: (a) Substernal chest pain or discomfort that is (b) provoked by exertion or emotional stress and (c) relieved by rest and/or nitroglycerin.
Atypical (probable) angina is chest pain or discomfort that lacks one of the characteristics of definite/typical angina (1).
Non-anginal chest pain is chest pain/discomfort that meets one or none of the typical angina characteristics.
We would classify this patient as having typical (definite) angina. The Canadian Cardiovascular Society (CCS) classification can be used to further characterize his anginal symptoms (see Table (2)). He has CCS class II angina. His non-invasive testing showed ST depressions after 15 minutes on the Bruce Protocol. The Duke Treadmill Score (3) can be calculated as: Exercise time (minutes on the Bruce protocol) – (5 x maximum ST segment deviation in mm) – (4 x [0 = no angina pain; 1 = non-limiting pain; 2 = exercise limiting). Low-risk scores are considered to be ≥ 5, intermediate risk is -10 to 4, high risk ≤ -11. His score would be 5 (15 minutes – (5x 2 mm ST elevation), or low-risk.
His nuclear stress showed a small reversible perfusion defect of the left ventricle. This table (4) summarizes the risk categorization of non-invasive cardiac testing. We can classify him as having low-risk findings on non-invasive studies.
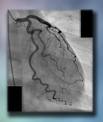
His coronary angiogram shows significant stenoses of his Right Coronary artery and Obtuse Marginal Branch of the Left Circumflex artery.
Summarizing the case, we have a 54 year old male with CCS class II angina (not on treatment), low-risk findings on non-invasive testing, and 2 vessel coronary artery disease (Obtuse marginal of L circumflex and R coronary artery).
The role of revascularization in this patient has been an area of intense research. Older studies compared Percutaneous Transluminal Coronary Angioplasty (PTCA or balloon angioplasty) to medical therapy in patients with stable angina. These studies (RITA-2, MASS II, VA ACME) all found similar rates of death in patients treated with PTCA compared with medical therapy. In fact, some of the studies found increased rates of MI in patients treated with PTCA compared with medical therapy (For example, RITA-2 randomized 1,018 patients to PTCA or medical therapy and found a non-significantly higher rate of death and MI after 5 years in the PTCA group: 9.4% vs. 7.6%) (5). However since this data was based on PTCA only (no stents), it is not as applicable to current practice.
There have been few large randomized studies examining PCI versus medical therapy in stable angina. The most applicable study is the Clinical Outcomes Utilizing Revascularization and Aggressive Drug Evaluation (COURAGE) trial, which randomized 2,287 subjects with stable coronary artery disease (CCS class I-III) to either revascularization (PCI) with aggressive medical therapy or aggressive medical therapy alone (6). Inclusion criteria was a 70% stenosis in at least one proximal epicardial coronary artery along with objective evidence of myocardial ischemia, or stenosis of 80% and classic angina without provocative testing. Relevant exclusion criteria included Left Ventricular dysfunction (EF < 30%) or a markedly positive stress test. The patient described in this case would have met the inclusion criteria for COURAGE. The study’s primary outcome was the composite of all-cause mortality and MI. After a mean follow-up period of 4.6 years, there was no difference in the primary outcome between the PCI group and medical therapy group (19.0% vs. 18.5% respectively).
Another recent study (BARI 2D trial (7)) examined the role of revascularization in diabetics with stable coronary artery disease (≥50% stenosis with positive stress test or ≥70% stenosis with angina). Physicians first decided what the revascularization procedure of choice would be, CABG or PCI. Subjects were than randomized to that procedure or optimal medical therapy. After an average follow up period of 5.3 years, survival did not differ between the revascularization and medical therapy groups (88.3% and 87.8% respectively). On further analysis, in the group deemed to require CABG, there were fewer MIs after CABG compared to medical therapy (10% 5-year rate of MI in the CABG group vs. 17% in medical therapy group; p-value 0.003) (8).
Based largely on this data recent appropriateness criteria for revascularization was released by a joint commission (American College of Cardiology Foundation). Pooled opinions from several experts in cardiology and cardiac surgery were used to determine the appropriateness of revascularization in several hypothetical situations (9). For each situation, revascularization was rated as appropriate, uncertain, or inappropriate. In this table we see some of those recommendations. For patients with 1-2 vessel disease, revascularization is rated as appropriate only when there are high-risk findings on non-invasive testing, intermediate-risk findings with symptoms on medical treatment, and low-risk findings with class III/IV symptoms on medical therapy. They rated revascularization as inappropriate when there is 1-2 vessel disease, low risk findings on non-invasive testing and class I/II symptoms off treatment, or intermediate risk findings on noninvasive testing without symptoms. For other situations with 1-2 vessel disease they rate revascularization as uncertain.
According to these guidelines and the data presented above, a treatment strategy of medical therapy alone (without revascularization) is appropriate in this patient with CCS class II angina (off medications), low-risk findings on non-invasive testing, and 1-2 coronary vessel disease (Answer choice B).
References
1. Gibbons RJ, Balady GJ, Bricker JT, Chaitman BR, Fletcher GF, Froelicher VF, Mark DB, McCallister BD, Mooss AN, O’Reilly MG, Winters WL, Jr., Antman EM, Alpert JS, Faxon DP, Fuster V, Gregoratos G, Hiratzka LF, Jacobs AK, Russell RO, Smith SC, Jr. ACC/AHA 2002 guideline update for exercise testing: summary article: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Update the 1997 Exercise Testing Guidelines). Circulation2002 Oct 1;106(14):1883-92. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=12356646
2. Campeau L. The Canadian Cardiovascular Society grading of angina pectoris revisited 30 years later. Can J Cardiol2002 Apr;18(4):371-9. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=11992130
3. Mark DB, Hlatky MA, Harrell FE, Jr., Lee KL, Califf RM, Pryor DB. Exercise treadmill score for predicting prognosis in coronary artery disease. Ann Intern Med1987 Jun;106(6):793-800. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=3579066
4. Gibbons RJ, Chatterjee K, Daley J, Douglas JS, Fihn SD, Gardin JM, Grunwald MA, Levy D, Lytle BW, O’Rourke RA, Schafer WP, Williams SV, Ritchie JL, Cheitlin MD, Eagle KA, Gardner TJ, Garson A, Jr., Russell RO, Ryan TJ, Smith SC, Jr. ACC/AHA/ACP-ASIM guidelines for the management of patients with chronic stable angina: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee on Management of Patients With Chronic Stable Angina). J Am Coll Cardiol1999 Jun;33(7):2092-197. http://www.sciencedirect.com/science?_ob=ArticleURL&_udi=B6T18-3WKY0RS-1R&_user=10&_rdoc=1&_fmt=&_orig=search&_sort=d&_docanchor=&view=c&_acct=C000050221&_version=1&_urlVersion=0&_userid=10&md5=0b375573db83ac15c73779b88f83cbcf
http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=10362225
5. Henderson RA, Pocock SJ, Clayton TC, Knight R, Fox KA, Julian DG, Chamberlain DA. Seven-year outcome in the RITA-2 trial: coronary angioplasty versus medical therapy. J Am Coll Cardiol2003 Oct 1;42(7):1161-70. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=14522473
6. Boden WE, O’Rourke RA, Teo KK, Hartigan PM, Maron DJ, Kostuk WJ, Knudtson M, Dada M, Casperson P, Harris CL, Chaitman BR, Shaw L, Gosselin G, Nawaz S, Title LM, Gau G, Blaustein AS, Booth DC, Bates ER, Spertus JA, Berman DS, Mancini GB, Weintraub WS. Optimal medical therapy with or without PCI for stable coronary disease. N Engl J Med2007 Apr 12;356(15):1503-16. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=17387127
7. Frye RL, August P, Brooks MM, Hardison RM, Kelsey SF, MacGregor JM, Orchard TJ, Chaitman BR, Genuth SM, Goldberg SH, Hlatky MA, Jones TL, Molitch ME, Nesto RW, Sako EY, Sobel BE. A randomized trial of therapies for type 2 diabetes and coronary artery disease. N Engl J Med2009 Jun 11;360(24):2503-15. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=19502645
8. Chaitman BR, Hardison RM, Adler D, Gebhart S, Grogan M, Ocampo S, Sopko G, Ramires JA, Schneider D, Frye RL. The bypass angioplasty revascularization investigation 2 diabetes randomized trial of different treatment strategies in type 2 diabetes mellitus with stable ischemic heart disease: impact of treatment strategy on cardiac mortality and myocardial infarction. Circulation2009 Dec 22;120(25):2529-40. http://circ.ahajournals.org/cgi/content/full/120/25/2529
9. Patel MR, Dehmer GJ, Hirshfeld JW, Smith PK, Spertus JA. ACCF/SCAI/STS/AATS/AHA/ASNC 2009 Appropriateness Criteria for Coronary Revascularization: A Report of the American College of Cardiology Foundation Appropriateness Criteria Task Force, Society for Cardiovascular Angiography and Interventions, Society of Thoracic Surgeons, American Association for Thoracic Surgery, American Heart Association, and the American Society of Nuclear Cardiology: Endorsed by the American Society of Echocardiography, the Heart Failure Society of America, and the Society of Cardiovascular Computed Tomography. Circulation2009 Mar 10;119(9):1330-52. http://www.ncbi.nlm.nih.gov/entrez/query.fcgi?cmd=Retrieve&db=PubMed&dopt=Citation&list_uids=19131581

One comment on “Appropriateness for Revascularization in Stable Angina”
Comments are closed.