Faculty Peer Reviewed
Measles remains one of the leading causes of preventable child mortality worldwide, despite the development of an effective vaccine in the 1960s. Even as late as the early 1990s, measles continued to infect tens of millions of people and claimed over a million lives each year (51]. Although mortality dropped by 78% from 2000 to 2008 due to aggressive control initiatives, the disease is still responsible for 164,000 deaths annually [12, 72]. Morbidity and mortality is mostly due to measles-associated pneumonia [13, 59], middle-ear infection [13, 30, 59], corneal inflammation and ulceration (27, 28, 46, 64), diarrhea [19, 35, 61, 70] and, rarely, subacute sclerosing panencephalitis [36, 37, 77].
Currently, the disease accounts for 3-4% of all deaths worldwide in children under the age of five, over half of which occur in sub-Saharan Africa [5, 74]. This region and the South-East Asia region are the two areas that are most struggling with measles control [75]. In addition to the widespread conflicts, enormous populations and persistent impoverishment that have debilitated immunization campaigns in these two regions, effective global measles control and elimination must also overcome a number of challenges posed by technical aspects of the vaccine, the clinical course of the disease and recent social issues.
Technical challenges of the measles vaccine include heat- and light-sensitivity [1, 3, 79]. Measles vaccines are stable for two years at 2-8°C and for one month at 25-30°C [1]. Above 37°C (98.6°F), however, the vaccine is inactivated within one hour. Unfortunately, nearly every country struggling with measles control is located in the tropics and regularly experiences temperatures much higher than 37°C [75], thus necessitating continuation of the cold chain for mobile vaccination units.
However, the main technical challenge of measles control programs is deciding the timing of the first dose. Infants are protected by passive maternal antibodies until 6-9 months after birth, during which time immunization is not possible [62]. If the vaccine is administered too early, it is ineffective and leads to a large percentage of susceptible individuals. If the vaccine is administered too late, there is a chance of widespread outbreaks occurring in the window of time between loss of maternal antibody and vaccination. Countries usually plan their first dose in respect to the status of the disease in the region. If measles incidence is high, the first dose is given at 9 months or sometimes as early as 6 months [20, 25]. If measles incidence is low, the first dose is administered between 12 to 15 months of age [15, 56]. Such is the case in the United States [14, 49], where measles vaccine is required in every state for grade school and/or college entry requirements [55]. A second dose of vaccine is administered to cover the 3-5% who fail to develop immunity after the first dose [48, 60], a minority which has played a very significant role in measles outbreaks [48]. While in the United States this dose is given between 4-6 years of age [14], countries with high measles prevalence can administer the second dose as early as one month after the first dose [11].
Several important challenges exist today that were either largely or wholly absent in past decades. First is the increased frequency and ease of regional and global travel. Primarily, this factor amplifies the spread of measles within susceptible areas. Areas in developing countries where measles is locally extinct are not free of the burden of the virus since importation of the disease can quickly reestablish indigenous transmission and trigger outbreaks [26].
Additionally, countries that have entirely eliminated measles are required to continuously maintain high vaccination coverage in their populations. Recent outbreaks in Western Europe [2, 38, 40, 63], Canada [7, 45] and the United States [9, 16, 57, 78], including 2008 and 2009 outbreaks in Brooklyn [34, 80], are a testament to this obligation. While measles vaccine has always been recommended for Americans travelling abroad [58], a large outbreak in South Africa, host of the 2010 World Cup, has underscored the importance of immunization to measles [8, 10].
In addition to these challenges, coverage in industrialized countries is not as simple as it may seem. In 1998, a study seemed to suggest a link between MMR vaccine and both autism and inflammatory bowel disease [71]. Coverage rates fell dramatically in the United Kingdom (where the study was conducted) from highs of near 90% in 1994 to <80% by the end of 1998 [39]. Levels remained as low as 79% until 2004 [47], much lower than the 95% necessary for effective herd immunity [31, 76]. Declines in coverage were also reported in various regions in the United States and Western Europe.
Despite countless studies showing no correlation and reports from the World Health Organization, the Centers for Disease Control and Prevention, the National Institutes of Health and the United Kingdom’s National Health Service to the same effect [17, 53, 54, 73], the shaken confidence has yet to fully recover. As of 2009, coverage rates in the United Kingdom stood at 82-84% in children under the age of two and 75% in children under the age of five [4, 47]. Activist groups against the MMR vaccine are persistent even though the author of the study has been accused of fixing his data [22] and charged with professional misconduct [24], as he had been paid £400,000 before the 1998 study by a legal group trying to sue vaccine companies for the alleged ill effects of the MMR vaccine [23]. In 2004, 10 of the original 13 authors issued a retraction of their interpretations presented in the article [50].
Recently, the General Medical Council of the United Kingdom condemned the manner in which the study was undertaken as dishonest, irresponsible and misleading [21, 33, 69], and The Lancet, which originally published the work, issued a full retraction of the paper [67]. On May 24, 2010, the author was formally stricken off the medical register in the United Kingdom [6, 32, 68].
Apart from these challenges, attempts at measles control must also deal with issues specific to the measles virus. Most candidates for control and elimination are compared to smallpox and the successful global smallpox eradication campaign. The measles virus has several biological characteristics that are advantageous to attempts at control. Like smallpox (and polio), there is no animal reservoir for the measles virus. The presence of animal reservoirs, which exist in diseases such as malaria, rabies, cholera and influenza, make eradication very difficult, as eradication would necessitate pathogen elimination from the animal reservoir as well. The lack of an animal reservoir means that all efforts can be aimed at disease transmission between humans.
Also like smallpox, a measles infection confers life-long immunity. The lack of reinfection results in a smaller population of susceptible individuals and therefore both slower and more limited transmission. Finally, molecular and structural constraints restrict mutation of the measles virion’s surface epitopes, allowing for continuous use of the current vaccines for many decades [29]. This is in stark contrast to viruses like influenza whose vaccines must be updated yearly due to high levels of surface molecular alterations [66]. As RNA viruses, both measles and influenza have high rates of genetic mutation, but only measles is limited structurally.
Other factors related to the clinical course of a measles infection, however, make the disease difficult to control. First, measles is highly contagious. The R0 value of the virus, which measures the average number of secondary infections resulting from a single primary case in a completely naïve (susceptible) population, is 12-18. In contrast, polio and smallpox both have values of 5-7. This infectivity can also be analyzed in terms of household members that will contract the disease from a single infected individual. In the case of measles, this figure is 75% [18, 43]; similar studies for smallpox have yielded figures between 19-36% [41, 44, 65]. In addition to increased numbers of cases, higher household incidence has been correlated to higher mortality [52], presumably because familial resources are overwhelmed in trying to care for the infected family members.
One of the benefits of the clinical course of smallpox infection is that the infectivity of the individual begins when the rash appears. In contrast, individuals infected by measles are most contagious three days before the appearance of rash [59]. This characteristic of measles contributes partly to its high R0 value and also to its high household infectivity rate. Those infected by smallpox, on the other hand, can be quickly targeted by quarantine and care before the disease is transmitted. In the smallpox eradication campaigns in central Africa, researchers observed that infected individuals would retreat to their villages and stay home when the rash appeared, limiting contact of the individual to the household and therefore yielding a lower RÂÂ0 than expected [42]. Measles presents a more intricate challenge.
Therefore, while global measles elimination is theoretically possible, it will be significantly more difficult than the successful example of smallpox eradication. Key differences between the diseases biologically and clinically, as well as technical challenges specific to the measles vaccine, virtually ensure that the disease will continue to take a global toll for years to come. It is essential to appreciate the obstacles to measles control if this burden is to be further reduced.
Taher Modarressi is a second year medical student at NYU School of Medicine
Peer reviewed by Melanie Maslow, Infectious Diseases, Section Editor, Clinical Correlations
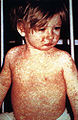
Image courtesy of Wikimedia Commons.
References:
[1] Arya, S. C., and N. Agarwal. 2004. Efficacy of measles vaccine interlinked with potency and storage. Acta Tropica 90:223-225.
[2] Atkinson, P., C. Cullinan, J. Jones, G. Fraser, and H. Maguire. 2005. Large outbreak of measles in London: reversal of health inequalities. Arch Dis Child 90:424-425.
[3] Bishai, D. M., S. Bhatt, L. T. Miller, and G. F. Hayden. 1992. Vaccine Storage Practices in Pediatric Offices. Pediatrics 89:193-196.
[4] British Broadcasting Channel. 17 April 2009. Jab reminder after measles cases, BBC News, available at http://news.bbc.co.uk/2/hi/uk_news/england/tees/8005294.stm.
[5] Bryce, J., C. Boschi-Pinto, K. Shibuya, and R. E. Black. 2005. WHO estimates of the causes of death in children. The Lancet 365:1147-1152.
[6] Burns, J. F. 24 May 2010. British Medical Council Bars Doctor Who Linked Vaccine With Autism, New York Times, available at http://www.nytimes.com/2010/05/25/health/policy/25autism.html.
[7] Canadian Broadcasting Corporation. 30 March 2010. Measles outbreak hits unvaccinated in B.C., CBC News, available at http://www.cbc.ca/canada/british-columbia/story/2010/03/30/bc-measles-outbreak.html.
[8] Â Centers for Disease Control and Prevention. 22 April 2010. 2010 Measles Update, Travelers’ Health, available at http://wwwnc.cdc.gov/travel/content/in-the-news/measles.aspx.
[9] Centers for Disease Control and Prevention. 2004. Brief Report: Imported Measles Case Associated with Nonmedical Vaccine Exemption — Iowa, March 2004. MMWR 53:1-2.
[10] Centers for Disease Control and Prevention. 2010. CDC Urges Awareness of Measles in South Africa, available at http://www.cdc.gov/measles/travel-worldcup.html.
[11]Â Centers for Disease Control and Prevention. 1994. General Recommendations on Immunization: Recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR 43(RR-1):1-48.
[12] Centers for Disease Control and Prevention. 2009. Global Measles Mortality, 2000-2008. MMWR 58:1321-1326.
[13] Centers for Disease Control and Prevention. 2008. Measles, p. 129-148. In W. Atkinson, J. Hamborsky, L. McIntyre, and S. Wolfe (ed.), Epidemiology and Prevention of Vaccine-Preventable Diseases, 10 ed. Public Health Foundation, Washington D.C.
[14]Â Centers for Disease Control and Prevention. 1998. Measles, Mumps, and Rubella – Vaccine Use and Strategies for Elimination of Measles, Rubella, and Congential Rubella Syndrome and Control of Mumps: Recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR 47(RR-8):1-57.
[15] Centers for Disease Control and Prevention. 2009. Recommended Immunization Schedules for Persons Aged 0 Through 18 Years – United States, 2009. MMWR 57:Q1-Q4.
[16] Centers for Disease Control and Prevention. 2008. Update: Measles — United States, January – July 2008. MMWR 57:893-896.
[17] Centers for Disease Control and Prevention. Vaccine Safety, Measles, Mumps, and Rubella (MMR) Vaccine, available at http://www.cdc.gov/vaccinesafety/Vaccines/MMR/MMR.html.
[18] Chapin, C. V. 1925. Measles in Providence, Rhode Island, 1858-1923. American Journal of Hygiene 5:635-655.
[19] Ciofi degli Atti, M. L., A. Filia, M. Massari, R. Pizzuti, L. Nicoletti, A. D’Argenzio, E. de Campora, A. Marchi, A. Lombardo, and S. Salmaso. 2006. Assessment of measles incidence, measles-related complications and hospitalisations during an outbreak in a southern Italian region. Vaccine 24:1332-1338.
[20] Cutts, F. T., M. Grabowsky, and L. E. Markowitz. 1995. The effect of dose and strain of live attenuated measles vaccines on serological responses in young infants. Biologicals 23:95-106.
[21] Deer, B. 31 January 2010. ‘Callous, unethical and dishonest’: Dr Andrew Wakefield, The Sunday Times. London, United Kingdom, available at http://www.timesonline.co.uk/tol/news/uk/health/article7009882.ece.
[22] Deer, B. 8 February 2009. MMR doctor Andrew Wakefield fixed data on autism, The Sunday Times. London, United Kingdom, available at http://www.timesonline.co.uk/tol/life_and_style/health/article5683671.ece.
[23] Deer, B. 31 December 2006. MMR doctor given legal aid thousands, The Sunday Times. London, United Kingdom, available at http://www.timesonline.co.uk/tol/news/uk/article1265373.ece.
[24] Deer, B. 11 September 2005. MMR scare doctor faces list of charges, The Sunday Times. London, United Kingdom, available at http://www.timesonline.co.uk/tol/news/uk/article565188.ece.
[25] Expanded Programme on Immunization (World Health Organization). 1990. Measles immunization before 9 months of age. Weekly Epidemiological Record 65:8-9.
[26] Ferrari, M. J., R. F. Grais, N. Bharti, A. J. K. Conlan, O. N. Bjornstad, L. J. Wolfson, P. J. Guerin, A. Djibo, and B. T. Grenfell. 2008. The dynamics of measles in sub-Saharan Africa. Nature 451:679-684.
[27] Â Foster, A., and A. Sommer. 1986. Childhood blindness from corneal ulceration in Africa: causes, prevention, and treatment. Bull World Health Organ 64:619-23.
[28] Foster, A., and A. Sommer. 1987. Corneal ulceration, measles, and childhood blindness in Tanzania. Br J Ophthalmol 71:331-343.
[29] Frank, S., and R. Bush. 2007. Barriers to antigenic escape by pathogens: trade-off between reproductive rate and antigenic mutability. BMC Evolutionary Biology 7:229.
[30] Gardiner, W. T. 1924. Otitis Media in Measles. The Journal of Laryngology & Otology 39:614-617.
[31] Gay, N. J. 2004. The Theory of Measles Elimination: Implications for the Design of Elimination Strategies. Journal of Infectious Diseases 189:S27-S35.
[32] General Medical Council. 24 May 2010. Determination on Serious Professional Misconduct and sanction – Dr. Andrew Jeremy Wakefield, available at http://www.gmc-uk.org/Wakefield_SPM_and_SANCTION.pdf_32595267.pdf.
[33] General Medical Council. 28 January 2010. Fitness to Practise Panel Hearing – Dr Andrew Jeremy Wakefield, available at http://www.gmc-uk.org/static/documents/content/Wakefield__Smith_Murch.pdf.
[34] Grady, D. 2 May 2008. Measles in U.S. at Highest Level Since 2001, New York Times, available at http://www.nytimes.com/2008/05/02/health/02measles.html.
[35] Greenberg, B. L., R. B. Sack, E. Salazar-Lindo, E. Budge, M. Gutierrez, M. Campos, A. Visberg, R. Leon-Barua, A. Yi, D. Maurutia, and et al. 1991. Measles-associated diarrhea in hospitalized children in Lima, Peru: pathogenic agents and impact on growth. J Infect Dis 163:495-502.
[36] Griffin, D. E. 2007. Measles Virus, p. 1551-1586. In D. M. Knipe and P. M. Howley (ed.), Fields’ Virology, vol. 2. Lippincott Williams & Wilkins, Philadelphia.
[37] Â Halsey, N. A., J. F. Modlin, J. T. Jabbour, L. O. N. Dubey, D. L. Eddins, and D. D. Ludwig. 1980. Risk factors in subacute sclerosing panencephalitis: a case-control study. Am. J. Epidemiol. 111:415-424.
[38] Hanratty, B., T. Holt, E. Duffell, W. Patterson, M. Ramsay, J. M. White, L. Jin, and P. Litton. 2000. UK measles outbreak in non-immune anthroposophic communities: the implications for the elimination of measles from Europe. Epidemiology and Infection 125:377-383.
[39] Health Protection Agency. 1999. MMR vaccine coverage falls in the United Kingdom. Commun Dis Rep Wkly 9:37.
[40] Health Protection Surveillance Centre. 2007. Annual Report 2006, p. 16-18. Health Protection Surveillance Centre (HPSC), Dublin, Ireland.
[41] Heiner, G. G., N. Fatima, and F. R. J. McCrumb. 1971. A study of intrafamilial transmission of smallpox. Am. J. Epidemiol. 94:316-326.
[42] Henderson, D. A. 2009. Presented at the lecture entitled “Smallpox Eradication”, Princeton University, Princeton, NJ, 27 March 2009.
[43] Hope-Simpson, R. E. 1952. Infectiousness of communicable diseases in the household: (measles, chickenpox, and mumps). The Lancet 260:549-554.
[44]Â Hopkins, D., J. Koplan, A. Hinman, and J. M. Lane. 1982. The case for global measles eradication. The Lancet 319:1396-1398.
[45] International SOS. 4 June 2010. Measles outbreaks in Vancouver area, British Columbia and Calgary, Alberta, Canada Country Guide, available at http://www.internationalsos.com/countryguide/medicalalerts.aspx?languageid=ENG&dnpid=34&reportid=27804.
[46] Kayikcioglu, O., E. Kir, M. Soyler, C. Guler, and M. Irkec. 2000. Ocular findings in a measles epidemic among young adults. Ocular Immunology & Inflammation 8:59-62.
[47] Laurance, J. 21 June 2008. Official warning: Measles ‘endemic’ in Britain, The Independent. London, available at http://www.independent.co.uk/life-style/health-and-wellbeing/health-news/official-warning-measles-endemic-in-britain-851584.html.
[48] Mathias, R. G., W. G. Meekison, T. A. Arcand, and M. T. Schechter. 1989. The Role of Secondary Vaccine Failures in Measles Outbreaks. American Journal of Public Health 79:475-478.
[49] Merck & Co. Inc. February 2006. Attenuvax Product Sheet, available at http://www.merck.com/product/usa/pi_circulars/a/attenuvax/attenuvax_pi.pdf.
[50] Murch, S. H., A. Anthony, D. H. Casson, M. Malik, M. Berelowitz, A. P. Dhillon, M. A. Thomson, A. Valentine, S. E. Davies, and J. A. Walker-Smith. 2004. Retraction of an interpretation. The Lancet 363:750-750.
[51] Murray, C. J. L., and A. D. Lopez. 1997. Mortality by cause for eight regions of the world: Global Burden of Disease Study. The Lancet 349:1269-1276.
[52] Â Nandy, R., T. Handzel, M. Zaneidou, J. Biey, R. Z. Coddy, R. Perry, P. Strebel, and L. Cairns. 2006. Case-Fatality Rate during a Measles Outbreak in Eastern Niger in 2003. Clinical Infectious Diseases 42:322-328.
[53] National Health Service. 2008. MMR and autism. National Health Service, United Kingdom, available at http://www.immunisation.nhs.uk/Vaccines/MMR/The_vaccine/mmr_autism.
[54] Â National Institute of Child Health and Human Development. 2006. Is there a link between autism and vaccines? National Institutes of Health, available at http://www.nichd.nih.gov/publications/pubs/autism/QA/sub4.cfm.
[55] National Network for Immunization Information. 2010. State Vaccine Requirements for School Entry, available at http://www.immunizationinfo.org/vaccines/state-requirements.
[56] Orenstein, W. A., L. Markowitz, S. R. Preblud, A. R. Hinman, A. Tomasi, and K. J. Bart. 1986. Appropriate age for measles vaccination in the United States. Dev Biol Stand 65:13-21.
[57] Parker, A. A., W. Staggs, G. H. Dayan, I. R. Ortega-Sanchez, P. A. Rota, L. Lowe, P. Boardman, R. Teclaw, C. Graves, and C. W. LeBaron. 2006. Implications of a 2005 Measles Outbreak in Indiana for Sustained Elimination of Measles in the United States. N Engl J Med 355:447-455.
[58] Parker, A. A., and A. Uzicanin. 2009. The Pre-Travel Consultation: Measles (Rubeola). In G. W. Brunette, P. E. Kozarsky, A. J. Magill, and D. R. Shlim (ed.), CDC Health Information for International Travel 2010. Mosby, Inc., available at http://wwwnc.cdc.gov/travel/yellowbook/2010/chapter-2/measles.aspx.
[59] Perry, R. T., and N. A. Halsey. 2004. The Clinical Significance of Measles: A Review. The Journal of Infectious Diseases 189:S4-S16.
[60] Poland, G. A., R. M. Jacobson, A. M. Thampy, S. A. Colbourne, P. C. Wollan, J. J. Lipsky, and S. J. Jacobsen. 1997. Measles reimmunization in children seronegative after initial immunization. JAMA 277:1156-1158.
[61] Pongrithsukda, V., K. Phonboon, and K. Manunpichu. 1986. Measles-associated diarrhoea in northeastern Thailand. Southeast Asian Journal of Tropical Medicine & Public Health 17:43-7.
[62] Reilly, C. M., J. Stokes, Jr., E. B. Buynak, H. Goldner, and M. R. Hilleman. 1961. Living attenuated measles-virus vaccine in early infancy. Studies of the role of passive antibody in immunization. N Engl J Med 265:165-9.
[63] Richard, J., V. Masserey-Spicher, S. Santibanez, and A. Mankertz. 2008. Measles outbreak in Switzerland–an update relevant for the European football championship (EURO 2008). Euro Surveill 13.
[64] Semba, R. D., and M. W. Bloem. 2004. Measles blindness. Survey of Ophthalmology 49:243-255.
[65] Sommer, A., and S. O. Foster. 1974. The 1972 smallpox outbreak in Khulna Municipality, Bangladesh: I. Methodology and epidemiologic findings. Am. J. Epidemiol. 99:291-302.
[66] Stohr, K. 2003. The WHO Global Influenza Program and Its Animal Influenza Network. Avian Diseases 47:934-938.
[67] The Editors of The Lancet. 2 February 2010. Retraction—Ileal-lymphoid-nodular hyperplasia, non-specific colitis, and pervasive developmental disorder in children, The Lancet, available at http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(10)60175-4/fulltext.
[68] Triggle, N. 24 May 2010. MMR doctor struck off register, British Broadcasting Channel, available at http://news.bbc.co.uk/2/hi/health/8700611.stm.
[69] Triggle, N. 28 January 2010. MMR scare doctor ‘acted unethically’, panel finds, British Broadcasting Channel, available at http://news.bbc.co.uk/2/hi/health/8483865.stm.
[70] Varavithya, W., S. Aswasuwana, P. Phuapradit, S. Louisirirotchanakul, S. Supavej, and S. Nopchinda. 1989. Etiology of diarrhea in measles. Journal of the Medical Association of Thailand 72 Suppl 1:151-4.
[71] Wakefield, A. J., S. H. Murch, A. Anthony, J. Linnell, D. M. Casson, M. Malik, M. Berelowitz, A. P. Dhillon, M. A. Thomson, P. Harvey, A. Valentine, S. E. Davies, and J. A. Walker-Smith. 1998. Ileal-lymphoid-nodular hyperplasia, non-specific colitis, and pervasive developmental disorder in children. Lancet 351:637.
[72] Â World Health Organization. 2009. Global reduction in measles mortality 2000-2008 and the risk of measles resurgence. Weekly Epidemiological Record 84:505-516.
[73] World Health Organization. 2001. Recent concerns regarding MMR vaccine, statement WHO/02. World Health Organization, available at http://www.who.int/inf-pr-2001/en/state2001-02.html.
[74] World Health Organization. 2008. World Health Statistics 2008. WHO Press, Geneva.
[75] World Health Organization, and UNICEF. 2005. Global Plan for Reducing Measles Mortality 2006-2010. World Health Organization, Geneva, Switzerland.
[76] Â World Health Organization, and UNICEF. 2001. Measles mortality reduction and regional elimination: strategic plan 2001-2005. World Health Organization, Geneva, Switzerland.
[77] Yalaz, K., B. Anlar, Y. Renda, S. Aysun, M. Topcu, and E. Ozdirim. 1988. Subacute Sclerosing Panencephalitis in Turkey: Epidemiological features. J Trop Pediatr 34:301-305.
[78] Yeung, L. F., P. Lurie, G. Dayan, E. Eduardo, P. H. Britz, S. B. Redd, M. J. Papania, and J. F. Seward. 2005. A Limited Measles Outbreak in a Highly Vaccinated US Boarding School. Pediatrics 116:1287-1291.
[79] Yuan, L., S. Daniels, M. Naus, and B. Brcic. 1995. Vaccine storage and handling. Knowledge and practice in primary care physicians’ offices. Can Fam Physician 41:1169-76.
[80] Â Zucker, J. R., and C. M. Zimmerman. 2009. Measles in Brooklyn. New York City Department of Health and Mental Hygiene, available at http://www.nyc.gov/html/doh/downloads/pdf/cd/2009/09md25.pdf.