Faculty Peer Reviewed
 Once thought to be exclusively the domain of gang members, prisoners, and those in the military, tattoos are now increasingly popular with the general population. The increasing visibility of tattoos on high-profile individuals such as athletes, musicians, and actors, combined with the increasing acceptability of tattoos among professionals, have made tattoos a common part of modern culture. Nevertheless, tattoo artists are subject to little regulation, and tattoo art comes with some real health risks. With an estimated 15% of Americans having at least one tattoo, it is important for the physician to be familiar with the safety and health risks of the tattooing process.
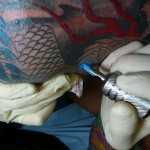
 The most common health hazard associated with tattooing is localized skin infection caused by Staphylococcus aureus (with some cases of community-acquired methicillin-resistant S. aureus reported) or Pseudomonas aeruginosa. Infection arises from the procedure itself, which requires piercing the skin. The tattooing process uses a needle that is controlled by an electromagnetic coil, enabling it to oscillate at a frequency between 80 to 150Hz. The needle punctures the skin at a depth of 1-4 millimeters, carrying the dye into the dermis, where it is then engulfed by macrophages. As the damaged skin heals, granulation tissue forms, and the dye remains permanently trapped in fibroblasts in the superficial dermis. The same process that introduces the dye can introduce the common bacteria noted above, causing infection. Physicians should remind their patients that tattooing is an invasive procedure and that the same precautions that are taken after getting a scrape or cut should be taken after obtaining a tattoo. A thorough washing of the tattoo site with soap and water is usually effective in preventing localized skin infection.
 Tattooing can also cause systemic infections such as staphylococcal toxic shock syndrome, pseudomonal abscesses, and infective endocarditis.  The British Cardiac Society/Royal College of Physicians and 60% of physician members of the International Society of Adult Congenital Cardiac Disease (IASCCD) surveyed in 1999 recommend prophylactic antibiotics before obtaining a tattoo for patients with congenital heart disease, as a preventive measure against infective endocarditis. Importantly, 75% of the same group of IASCCD physicians surveyed disapprove outright of tattoos for their patients with congenital heart disease. Â
 Tattooing has also caused tetanus, tuberculosis, hepatitis B, and hepatitis C. Patients who are considering tattoos should ensure that their tetanus and hepatitis B vaccines are up to date. Similarly, baseline testing for hepatitis and HIV may be done for patient reassurance or, if results are positive, as cautionary information for the tattoo artist. Finally, while there have been no clear cases of HIV having been caused by tattooing, there is the potential for HIV infection. The risk for all these diseases can be lowered if tattoo artists use new needles with each patient and pour new ink into a well for each patient so as not to “double-dip†needles from different patients into the same inkwell.
 Hypersensitivity reactions can be caused by the introduction of foreign ink into the dermis. Tattoo inks do not need FDA approval and can contain a wide variety of ingredients that can cause skin reactions. While aluminum, oxygen, titanium, and carbon are the most common elements of tattoo ink and have been found to be safe, mercury, chromium, cadmium, and cobalt are also commonly used and have all been associated with delayed hypersensitivity reactions. Corticosteroids can be used to treat patients who develop hypersensitivity reactions in response to tattoos. Finally, while rare, there have been some reported cases of anaphylaxis associated with tattooing.
 Because some inks contain high levels of iron oxide, there is the potential for burns or distortions of the tattoo caused by magnetic hysteresis during magnetic resonance imaging (MRI). Nevertheless, tattoos are generally not a contraindication for having an MRI procedure. Because adverse hypersensitivity and MRI events are associated with inks that contain mercury, chromium, cadmium, and cobalt and higher levels of iron oxide, physicians can advise patients to ask their tattoo artist to use an ink that is low in these materials.
 Of course, many of the risks are in the control of the tattoo artist rather than the person receiving the tattoo. Tattoos can be obtained in a wide variety of places, ranging from luxury hotel studios in Las Vegas to side-of-the-road tents at state fairs, with a wide range of hygiene. While no site can be guaranteed safe–the NYC Dept. of Health licenses tattoo artists, not parlors–choosing a professional studio likely decreases the risk of infections and could be recommended to patients. In addition to changing needles and inkwells, it is also a good idea for patients to ensure that the tattoo artist washes his hands and changes gloves between each client, disinfects all equipment, shaves and cleans the body site with an antimicrobial wash before administering the tattoo, and provides appropriate aftercare instructions. The tattoo artist should also be educated about potential health risks and adverse events associated with tattoos, as clients might return to the tattoo artist before going to a physician if they experience a problem.
 While the risks may be small, the popularity of tattoos in our culture has greatly increased the likelihood that physicians will deal with health issues involving tattoos. These health issues can range from mild irritations to serious lifelong diseases, some of which can be prevented or treated and some of which cannot. Regulations for tattoo artists, while generally loose, vary by state and can affect the risks involved. A physician should be prepared to address these issues, offering information, advice, preventive measures, and treatment.
 Farzon A. Nahvi is a 3rd year medical student at NYU School of Medicine
Peer reviewed by Demetre Daskalakis, MD, Department of Medicine (Infectious Disease) NYU Langone Medical Center
Image courtesy of Wikimedia Commons
References:Â
1. Armstrong ML, McConnell C. Tattooing in adolescents: more common than you think–the phenomenon and risks. J Sch Nurs. 1994;10(1):26-33.
 2. Armstrong ML. Tattooing, body piercing, and permanent cosmetics: a historical and current view of state regulations, with continuing concerns. J Environ Health. 2005; 67(8):38-43,54,53.
 3. Centers for Disease Control and Prevention (CDC). Methicillin-resistant Staphylococcus aureus skin infections among tattoo recipients–Ohio, Kentucky, and Vermont, 2004-2005.  MMWR;2006;55(24):677-9.
 4. Cetta F, Graham LC, Lichtenberg RC, Warnes CA. Piercing and tattooing in patients with congenital heart disease: patient and physician perspectives. J Adolesc Health. 1999;24(3):160-162.
 5. Delahaye F, Wong J, Mills PG. Infective endocarditis: a comparison of international guidelines. Heart. 2007;93(4):524-527.
 6. Dron P, Lafourcade MP, Leprince F, et al. Allergies associated with body piercing and tattoos: a report of the Allergy Vigilance Network. Eur Ann Allergy Clin Immunol. 2007;39(6):189-192.
 7. Farrow JA, Schwartz RH, Vanderleeuw J. Tattooing behavior in adolescence. A comparison study. Am J Dis Child. 1991;145(2):184-187.
 8. Hayes MO, Harkness GA. Body piercing as a risk factor for viral hepatitis: an integrative research review. Am J Infect Control. 2001;29(4):271-274.
 9. Kohut A, Parker K, Keeter S, Doherty C, Dimock M. How young people view their lives, futures and politics: a portrait of “Generation Next.†Pew Research Center 2007.
 10. Long GE, Rickman LS. Infectious complications of tattoos. Clin Infect Dis. 1994; 18(4):610-619.
 11. Mayers LB, Judelson DA, Moriarty BW, Rundell KW. Prevalence of body art (body piercing and tattooing) in university undergraduates and incidence of medical complications. Mayo Clin Proc. 2002;77(1):29-34.
 12. Mayo Clinic Foundation for Medical Education and Research. Tattoos: understand risks and precautions. http://www.mayoclinic.com/health/tattoos-and-piercings/MC00020/NSECTIONGROUP=2. Accessed on September 16, 2010.
 13. O’Malley CD, Smith N, Braun R, Prevots DR. Tetanus associated with body piercing. Clin Infect Dis. 1998;27(5):1343-1344.
 14. Wagle WA, Smith M. Tattoo-induced skin burn during MR imaging. AJR Am J Roentgenol. 2000;174(6):1795.

2 comments on “How Safe Is That Tattoo?”
Comments are closed.