Peer Reviewed
Former Mayor Michael Bloomberg’s proposal to limit sales of sugary drinks over 16 ounces was rejected by New York’s highest court this week [1]. Given that this was the final appeal, the soda ban is officially over. Although supporters hoped this would be a stepping-stone in the fight against obesity, opponents felt this proposal threatened consumer autonomy. While the soda ban had divided new Yorkers into several factions, one thing that most of us can support this week is the United States soccer team’s advancement to the World Cup quarterfinals despite a loss against Germany [2]. With the next round to look forward to, we also turn to some exciting new publications in the journals.
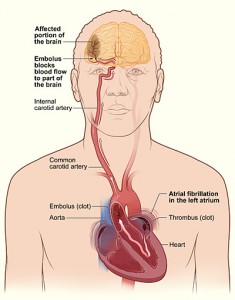
Monitoring for Atrial Fibrillation in Cryptogenic Stroke
This week two studies were published in The New England Journal of Medicine addressing monitoring for Atrial Fibrillation(AF) after cryptogenic stroke, or stroke due to unclear etiology without known carotid stenosis, documented atrial fibrillation, or stenotic intracranial vessels. The first, the EMBRACE trial, [3] randomized 572 patients with cryptogenic ischemic stroke or TIA to either a 30-day electrocardiogram monitoring with a portable event monitor or conventional 24-hour monitoring to detect AF. The primary outcome of this study was newly detected AF lasting 30 seconds or more within 90 days. AF was detected in 16.1% of patients as compared with 3.2% in the control group (p<0.001)(number needed to screen: 8). Even more impressive was the secondary outcome of patients on oral anticoagulation at 90 days (18.6% of the intervention group versus 11.1% of the control group). It appears that 30 day ECG monitoring, as opposed to the conventional 24 hour monitoring, allows higher detection rates of paroxysmal AF and thereby allows more appropriate initiation of oral anticoagulants for secondary prevention in these patients.
The second study, CRYSTAL AF, also compared screening methods for AF in patients with cryptogenic stroke or TIA [4]. Four-hundred-forty-one patients were randomized to receive long-term monitoring with an insertable cardiac monitor (ICM) versus conventional follow up with routine ECGs. At 6 months, AF was detected in 8.9% of the patients in the ICM group versus 1.4% of patients in the control group (hazard ratio, 6.4; 95% CI 1.9 to 21.7; P<0.001). At 12 months, 12.4% of patients with the ICM were detected to have AF vs. 2.0% in the conventionally monitored group (P<0.001). Although this data is compelling, the investigators point out that the process of ICM implantation is more invasive and not without risk of infection. These machines also have limited data memory and may overwrite previous data, thereby defeating the purpose of the longer-term monitoring.
An accompanying editorial in the NEJM, by Dr. Kamel Hooman, a neurologist at Weil Cornell Medical College, notes that although these articles elucidate the need for more prolonged cardiac monitoring after cryptogenic stroke, nearly two thirds of patients studied did not have AF as a source of their stroke [5]. Time intensive, and sometimes invasive efforts to search for AF may often be without reward. Further, anticoagulation for patients with subclinical AF is not well studied, particularly the stroke risk relative to the proportion of time in AF. He also brings up the question of the cost of implantable loop recorders in a large patient population, and instead suggests that external loop recorders such as those used in the EMBRACE trial be more widely used. These issues remain unexplored, but the significant findings in the data presented certainly make a compelling argument for more closely monitoring this patient population for AF.
The Use of 3-D Imaging in Breast Cancer Screening
While NEJM is published studies on AF, the Journal of the American Medical Association (JAMA) is tackling the hot topic of breast cancer prevention [6]. At a time when several celebrities, such as Angelina Jolie, are taking steps to minimize their cancer risks, many patients are asking how to do the same. This study attempts to answer the debate of digital versus 3-dimensional (3-D) breast imaging by suggesting that the addition of tomosynthesis, or 3-D imaging, increases cancer detection rates and decreases false positives. At 13 breast-centers, nearly 500,000 digital mammographies were examined before and after the use of tomosynthesis.. The addition of tomosynthesis was associated with an increased positive predictive value for recall (4.3% to 6.4% with tomosynthesis) and for biopsy (24.2% to 29.2% with tomosynthesis). Invasive cancer detection rates increased from 2.9 per 1000 screens with digital mammography to 4.1 per 1000 screens with both modalities. Although these results appear promising and the authors conclusively endorse use of tomosynthesis, there is still significant cost vs. benefit analysis that is needed before widespread implementation of tomosynthesis.
Colon Capsule vs CT Colonography After Incomplete Colonoscopy
Gut published a study comparing colon capsule endoscopy (CCE) to computed tomography colonography (CTC) in patients with incomplete colonoscopy [7]. The 4-15% of patients who have a suboptimal colonoscopy, often due to poor prep, generally undergo CTC to complete colonic evaluation per current guidelines. One hundred patients with previously incomplete colonoscopy were enrolled in this prospective study to undergo CCE or CTC. Overall the two tests were comparable in adequately assessing colonic pathology. CCE had greater relative sensitivity (2.0, 95% CI 1.34-2.98) for lesions greater than 6mm. For both tests, no cancers were missed at a mean clinical follow-up of 20 months. In centers where CCE is available, this study suggests that it is a safe and feasible method for improved colonic visualization following incomplete colonoscopy.
Other interesting articles in the news this week include:
High-dose simvastatin reduced the annual rate of whole-brain atrophy compared with placebo in patients with secondary progressive multiple sclerosis [8]. This advances the use of this treatment to phase 3 trials.
Deferring antiretroviral therapy after a diagnosis of cryptococcal meningitis for 5 weeks was found to be associated with improved survival as compared with initiating therapy at 1-2 weeks [9].
An interesting viewpoint article in JAMA discusses the contradictory nature of medical professionals participating in capital punishment [10].
Dana Zalkin is a 4th year medical student at NYU School of Medicine
Peer reviewed by Jessica Taff, MD, Chief Resident, NYU Langone Medical Center
Image courtesy of Wikimedia Commons
References:
1. Grynbaum, Michael. New York’s Ban on Big Sodas is Rejected by Final Court. http://www.nytimes.com/2014/06/27/nyregion/city-loses-final-appeal-on-limiting-sales-of-large-sodas.html?ref=todayspaper.  Published 6/26/2014.
2. Borden, Sam. U.S. Moves On With Assist From Portugal. http://www.nytimes.com/2014/06/27/sports/worldcup/world-cup-2014-us-germany-recife-brazil.html?src=me. Â Published 6/26/2014.
3. Gladstone et al. Atrial fibrillation in patients with cryptogenic stroke. N Engl J Med. 2014 Jun 26;370(26):2467-77. http://www.nejm.org/doi/full/10.1056/NEJMoa1311376
4. Sanna et al. Cryptogenic Stroke and Underlying Atrial Fibrillation. N Engl J Med. 2014 Jun 26;370(26):2478-2486. http://www.nejm.org/doi/full/10.1056/NEJMoa1313600
5. Kamel, H. Heart-Rhythm Monitoring for Evaluation of Cryptogenic Stroke. N Engl J Med. 2014 Jun 26;370(26):2532-2533. http://www.nejm.org/doi/full/10.1056/NEJMe1405046
6. Friedewald et al. Breast Cancer Screening Using Tomosynthesis in Combination with Digital Mammography. JAMA 2014 Jun 25;311(24):2499-2507. http://jama.jamanetwork.com/article.aspx?articleid=1883018
7. Spada et al. Colon Capsule Versus CT Colonography in Patients with Incomplete Colonoscopy: A Prospective, Comparative Trial. Gut 2014 Jun 24. [Epub ahead of print]. http://gut.bmj.com/content/early/2014/06/24/gutjnl-2013-306550.long
8. Chataway et al. Effect of high-dose simvastatin on brain atrophy and disability in secondary progressive multiple sclerosis (MS-STAT): a randomised, placebo-controlled, phase 2 trial. Lancet. 2014 Jun 28;383:2213-2221. http://www.sciencedirect.com/science/article/pii/S0140673613622424
9. Boulware et al. Timing of Antiretroviral Therapy after Diagnosis of Cryptococcal Meningitis. N Engl J Med. 2014 Jun 26;370(26):2487-2498. http://www.nejm.org/doi/full/10.1056/NEJMoa1312884
10. Truog RD, Cohen IG, Rockoff MA. Physicians, Medical Ethics, and Execution by Lethal Injection. JAMA. 2014 Jun 18;311(23):2375-2376. http://jama.jamanetwork.com/article.aspx?articleid=1874217