Vivian Hayashi MD, Robert Smith MD
The patient is an 82 year old man with frequent breathlessness. The patient had been admitted several times in the past two years for congestive heart failure. Two years earlier, the patient suffered an NSTEMI. A diagnostic cardiac catheterization revealed triple vessel coronary disease. A decision to perform CABG vs coronary stenting was delayed pending an evaluation of iron-deficiency anemia associated with a positive test for fecal occult blood. A recent echocardiogram showed normal left ventricular function but diastolic non-compliance. Treatment was begun with daily furosemide 80mg, along with lisinopril, carvedilol, nitrates and hydralazine. Of note, the patient was in atrial fibrillation treated with coumadin. The past medical history included diabetes, chronic kidney disease (baseline creatinine range, 2-3.5 mg/dl), a pontine embolic stroke with residual dysarthria and mild dysphagia, and a small hemorrhagic stroke with residual left hemiparesis. Social history was significant for heavy alcohol abuse and smoking many years earlier. Physical exam showed normal vital signs, unlabored respiration at rest, diminished breath sounds at the bases, and mild pitting edema.
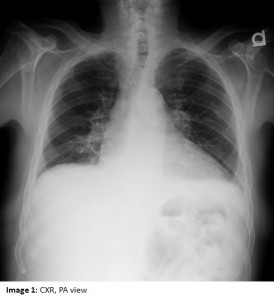
Chest radiograph is shown below.

One comment on “Mystery Quiz”
Comments are closed.