 By Arvind Reddy Devanabanda, MD
By Arvind Reddy Devanabanda, MD
Peer Reviewed
Americans are anxiously awaiting a Supreme Court ruling in King v. Burwell. In this case, the existence of federal subsidies for health insurance coverage in 34 states is at risk. If the Supreme Court rules against the administration, average premiums in some states could double and this may lead to thousands dropping out of their health plans, which would hurt both Democrats and Republicans, and more importantly, American health care in general [1]. This week, we also look at other American public health challenges, including improving outcomes from out-of-hospital cardiac arrests.
Can early bystander CPR increase survival in out-of-hospital cardiac arrests?
A recent Swedish study published in the NEJM examined the impact of cardiopulmonary resuscitation (CPR) performed in out-of-hospital settings prior to arrival of emergency medical services (EMS) [2]. This remains a significant public health challenge as there are 420,000 deaths every year in the United States from out-of-hospital cardiac arrests. While international guidelines have established the benefit of CPR overall, one criticism has been the lack of randomized clinical trials to show that bystander CPR is beneficial. This recent study evaluated if CPR initiated before arrival of EMS was associated with an increase in 30-day survival compared to delayed CPR, after accounting for confounding variables such as age, sex, location of cardiac arrest, cause of cardiac arrest, initial cardiac rhythm, EMS response time from collapse to call for EMS, and year of the event.
The study included all cases of EMS-treated and bystander-witnessed out-of-hospital cardiac arrests in the Swedish Cardiac Arrest Registry from 1990 to 2011. Cases witnessed only by EMS and non-witnessed cases were excluded. CPR was performed before the arrival of EMS in 15,512 (51%) of cases and was not performed in 14,869 (48.9%) of cases. The 30-day survival rate was 10.5%, with an odds ratio of 2.15 (95% confidence interval, 1.88 to 2.45) when CPR was performed before EMS arrival. This compared to a 30-day survival rate of 4.0% when CPR was not performed before EMS arrival. Also of interest, telephone -based CPR instructions were associated with increased 30-day survival rates. The results of this study suggest that bystander CPR does indeed save lives. It was also noted that patients who underwent CPR before EMS arrival were likely in settings outside of the home. It is possible that many in-home cardiac arrests are witnessed by persons not trained in CPR, such as the elderly or children. It is estimated that approximately 3 million out of 9 million Swedes are trained in CPR. The question that now remains is how we as a nation can educate more people on basic life support and CPR. Should it be part of the mandatory educational curriculum of high schools and work places?
How can pharmacists help physicians control blood pressure?
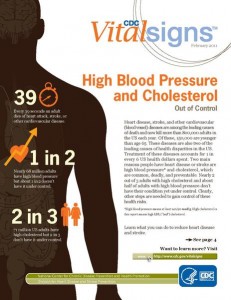
The scope of the practice of pharmacists continues to evolve, particularly in the management of medications related to blood pressure control [3]. Prior systematic reviews and meta-analyses have shown that with interventions by pharmacists, systolic blood pressures can decrease by as much as 7.6 points (95% confidence interval -9.5 to 6.3) [4]. Importantly, this effect was limited by the extent of physician follow-up [5]. A recent randomized controlled trial conduced in Alberta, Canada hypothesized that by allowing pharmacists to independently prescribe drug therapy, hypertension can be better controlled. This study enrolled 248 adults with high blood pressure as defined by Canadian guidelines through community pharmacies, hospitals, or primary care centers in 23 communities in Alberta [3]. Patients in the intervention group received an assessment of blood pressure and cardiac risk factors from their pharmacists, including education on hypertension, laboratory monitoring, and follow-up visits, while the control group received usual care from their pharmacist or primary care physician. The primary outcome was change in systolic blood pressure (SBP) at 6 months. Overall, the intervention group had a mean reduction in SBP of 18.3 points compared with 11.8 points in the standard treatment group, with an odds ratio in favor of achieving BP target of 2.32 (95% confidence interval 1.17 – 4.15). There were, however, several limitations to the study. Neither the patients nor the pharmacists were blinded to the intervention, the sample size was small, and the pharmacists received remuneration for their participation, whereas the physicians did not. Finally, the study does not report adverse outcomes from medication management either from pharmacist or physician prescriptions. Despite these limitations, this study does provide evidence that the use of interdisciplinary teams that includes pharmacists is useful in achieving blood pressure targets.
Cinacalcet and cardiovascular disease in hemodialysis.
A disruption in bone metabolism is a common complication of chronic kidney disease (CKD). Fibroblast growth factor 23 (FGF-23), a hormone secreted by osteocytes and osteoblasts, has been shown to be elevated in patients with CKD and is associated with adverse cardiovascular outcomes. In animal models, FGF 23 has been shown to induce cardiac muscle hypertrophy as well as fatal cardiac arrhythmia [6]. Among patients receiving hemodialysis (HD), the serum concentrations of FGF-23 are two to three times the normal limits [6]. However, until the current EVOLVE trial (The Evaluation of Cinacalcet HCl Therapy to Lower Cardiovascular Events), it was unknown whether reductions of FGF-23 can lead to improvement in cardiovascular and mortality outcomes [6]. In this study, the authors performed a secondary analysis of the EVOLVE trial comparing cinacalcet to conventional therapy to lower calcium levels in patients on HD with secondary hyperparathyroidism. Patients randomized to cinacalcet had a greater than 30% reduction in FGF-23 at week 20. This reduction in FGF-23 was associated with a nominally significant reduction in the death (HR 0.82, 95% CI 0.69-0.98), CV mortality (HR 0.66, 95% CI 0.50-0.87) and heart failure (HR 0.69, 95% CI 0.48-0.99). Overall, the study showed a nominal reduction in mortality associated with reductions of FGF23 levels and cinacalcet use and may suggest additional benefits of cinacalcet as well. However, association does not necessarily imply causation.
Other news in the journals:
Gastroenterology this week published a summary of recent advancements in the treatment of patients with co-infection of HIV and hepatitis C [7]. Also included in that same journal was an article describing how to achieve the fellowship of your choice, written from the perspective of several fellowship program directors [8].
Dr. Arvind Reddy Devanabanda is a 1st year resident at NYU Langone Medical Center
Peer reviewed by Dr. Karin Katz, Chief Resident, Internal Medicine at the VA Medical Center
Image courtesy of Wikimedia Commons
References:
1. The Health Care Supreme Court Case: Who would be Affected? New York Times. June 2, 2015. http://www.nytimes.com/interactive/2015/03/03/us/potential-impact-of-the-supreme-courts-decision-on-health-care-subsidies.html?_r=0
2. Hasselqvist. I, Riva G, Herlitz J et al. Early Cardiopulmonary Resuscitation in Out-of-Hospital Cardiac Arrest. New England Journal of Medicine. June 11, 2015. 372:2307-2315 http://www.nejm.org/doi/full/10.1056/NEJMoa1405796
3. Tsuyuki R, Houle S, Charrois T et al. A Randomized Trial of the Effect of Pharmacist Prescribing on Improving Blood Pressure in the Community: The Alberta Clinical Trial in Optimizing Hypertension (RxACTION). Circulation. Published Before Print. http://circ.ahajournals.org/content/early/2015/06/10/CIRCULATIONAHA.115.015464.abstract
4. Santashi V et al., Improving Blood Pressure Control Through Pharmacist Intervention: A meta-analysis of randomized control trials. Journal of American Heart Assoication. 2014 http://jaha.ahajournals.org/content/3/2/e000718.abstract
5. Altowaijri A et al., A systematic review of the clinical and economic effectiveness of clinical pharmacist intervention in secondary prevention of cardiovascular disease. Journal of Management Care Pharmacology. 2013 http://www.ncbi.nlm.nih.gov/pubmed/23697478
6. Moe et al. Cinacalcet, FGF23 and Cardiovascular disease in hemodialysis: The EVOLVE Trial. Circulation. Published before Print. http://circ.ahajournals.org/content/early/2015/06/09/CIRCULATIONAHA.114.013876.abstract
7. Paul Y Kwo, Saurabh Agrawal. HCV/ HIV coinfection: A new treatment paradigm. Gastroenterology. Published online April 29, 2015 http://www.ncbi.nlm.nih.gov/pubmed/25935524
8. Andrew Chan, Kathyrn Peterson. How to position for the gastroenterology fellowship of your choice: The Program director perspective http://www.gastrojournal.org/article/S0016-5085(15)00578-8/abstract
