 A 26 year old woman developed uncontrolled hypertension peripartum 5 years prior to this presentation After diagnosis she was intermittently compliant with her medication although remained asymptomatic. She now presents with new onset congestive heart failure. On admission, she was in mild respiratory distress. Her physical exam was notable for tachycardia with a blood pressure ranging from 160/100-200/110. She had a jugular-venous pressure of 8cm, +S4, crackles were present bilaterally 1/2 way up, but no peripheral edema. Labs were notable only for renal insufficiency (creatinine 1.5), but were otherwise unremarkable. Transthoracic echocardiogram revealed an ejection fraction of 20%, global hypokinesis, and a dilated left ventricle. Chest catscan was consistent with pulmonary edema.
A 26 year old woman developed uncontrolled hypertension peripartum 5 years prior to this presentation After diagnosis she was intermittently compliant with her medication although remained asymptomatic. She now presents with new onset congestive heart failure. On admission, she was in mild respiratory distress. Her physical exam was notable for tachycardia with a blood pressure ranging from 160/100-200/110. She had a jugular-venous pressure of 8cm, +S4, crackles were present bilaterally 1/2 way up, but no peripheral edema. Labs were notable only for renal insufficiency (creatinine 1.5), but were otherwise unremarkable. Transthoracic echocardiogram revealed an ejection fraction of 20%, global hypokinesis, and a dilated left ventricle. Chest catscan was consistent with pulmonary edema.
The patient was treated with diuretics and afterload reduction with improvement of her blood pressure and her respiratory distress. Our leading diagnosis was viral myocarditis and the cardiology consult recommended a cardiac MRI to further confirm this diagnosis. She will first undergo a cardiac catheterization to rule out an ischemic contribution.
Questions:
1. Assuming a normal catheterization and a diagnosis of non-ischemic dilated cardiomyopathy, what is the appropriate subsequent work-up?
2. What are the indications for endomyocardial biopsy?
3. Does cardiac MRI sufficiently rule out infiltrative disease (eg sarcoid, amyloid) to obviate the need for biopsy?
-Meera Malhotra, PGY-3
Commentary By: William Slater, MD Associate Professor of Medicine, Divsion of Cardiology
When thinking about a 26 year old woman with new onset symptoms of heart failure, the first question relates to the duration of left ventricular dysfunction-i.e. could this be myocarditis or, as is true most frequently, is this simply the onset of symptoms from a longer-standing cardiomyopathy. A useful guide in this regard is the size of the left ventricle (LV) and the left atrium (LA). While acute fulminate carditis can dilate the LV a bit, it generally does not give you a significantly dilated LV, since this takes time to develop. Even more useful, I think, is the LA size–it takes time for elevated left ventricular end diastolic pressure (LVEDP) to translate into LA stretch, so if LA size is significantly dilated (let’s say >4.5 cm if nl<4 cm), carditis is unlikely.
Something else I’ve found helpful sometimes in trying to assess the duration of a patient’s heart disease is reviewing the prior chest x-rays. Few people have old echocardiograms, but many people have old chest x-rays, perhaps from an old positive PPD, on immigration, from a primary MD’s office—and whether the LV and/or LA was enlarged on that film can help. That’s potentially useful in this case as well.
In the event that her heart is normal size or only mildly dilated with EF 20% and new CHF symptoms, carditis enters the picture. An ESR, CRP, CPK rise helps but is obviously insensitive and non-specific for the diagnosis. Viral etiologies include viral coxsackie and adenovirus which are most common, but HIV, herpes, Cytomegalovirus should also be considered. Viral IgM titers for these culprit pathogens can be useful. One should also consider lyme, rheumatic (if valvulitis is present as well) and uncommon etiologies (diphtheria, drugs, etc). Peripartum cardiomyopathy is probably an autoimmune carditis, though the etiology is not certain.We usually recommend a cardiac catheterization in a patient with congestive heart failure since myocardial viability can only really be discussed if one knows that there is a severe coronary stenosis supplying hypokinetic area and revascularization is one of the few things we can do which can make a big difference, but one can probably forego this here. MRI can suggest carditis and certainly can guide where to biopsy if that path is chosen, but MRI findings are non-specific.
Myocardial biopsy is generally not advocated unless the patient is in rapid acute decline (giant cell myocarditis is then a consideration–under 1% of cases but very responsive to immunosuppression). Since 1/3 of cases resolve, this spontaneous resolution rate mitigates against immunosuppressive treatment at first diagnosis, particularly since it is of unproven value. If the patient is in rapid decline, many centers will biopsy guided by MRI; there seem to be autoimmune features on biopsy which, in the retrospective analysis of myocarditis trials, predict a drug responsive group. What to do with the patients who neither get better nor decline is controversial–most centers will simply treat supportively, though some will biopsy at 3 months and treat the group with strong autoimmune features with cyclosporine and steroids. The largest myocarditis trial (Mason, et al, NEJM) showed no benefit to treatment, but the trial has been criticized for allowing entry of patients with symptoms up to several months, and there did seem to be a suggestion of benefit retrospectively in those whose biopsies showed strong autoimmune features. Other trials of immune modulation (gamma globulin infusion, for ex) have proven negative.
Our workup for etiology of cardiomyopathy (versus carditis) thus should include exclusion of CAD, HIV testing, TSH, exclusion of sarcoid (CXR, LFT’s-alkaline phosphatase, adenopathy, ACEI level although insensitive), ferritin, CPK (for some familial cardiomyopathies), and a history of alcohol and illicit or toxic drug use.
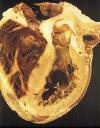
Image of dilated cardiomyopathy courtesy Images.md (NYU library licensed)

One comment on “How Do You Approach A Patient with a Non-Ischemic Cardiomyopathy”
Could you please tell me what specific labs should be ordered. Please email me back if possible.
Thank you
Comments are closed.