Commentary by Judith Brenner MD, Associate Program Director, NYU Internal Medicine Residency Program
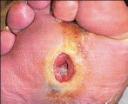
The most recent installment in JAMA’s Rational Clinical Exam Series seeks to determine the accuracy of the history, physical exam, radiology and laboratory in making the diagnosis of osteomyelitis in diabetics. This is relevant given its frequency of occurrence and its cost and since the gold standard for diagnosis, namely a bone biopsy and culture, is less than optimal for a variety of reasons.
 Less than 10% of the nearly 300 articles reviewed were included for review by the authors and of the 10%, most were graded in the mid categories for quality. Nonetheless, some important findings were reported (highlighted in green).
Less than 10% of the nearly 300 articles reviewed were included for review by the authors and of the 10%, most were graded in the mid categories for quality. Nonetheless, some important findings were reported (highlighted in green).
| Finding | Likelihood Ratio | Negative Likelihood Ratio |
| Ulcers >2 cm2 | 7.2 (CI 1.1-49) | 0.48 (CI 0.31-.076) |
| Positive “probe to bone” test* | 6.4 (CI 3.6-11) | 0.39 (CI 0.20-0.76) |
| ESR >70 | 11 (CI 1.6-79) | 0.34 (CI 0.06-1.9) |
| Abnormal plain X-ray** | 2.3 (CI 1.6-3.3) | 0.63 (CI 0.51-0.78) |
| Abnormal MRI | 3.8 (CI 2.5-5.8) | 0.14 (CI 0.08-0.26) |
*Probe to bone test: the examiner gently and in a sterile fashion, probes the ulcer with a steel probe to determine if the probe can advance to bone
**abnormal X-Ray findings include: focal loss of trabecular pattern, periosteal reaction, and frank bone destruction. 2 or 3 views can be selected
For example, the interpretation is as follows:
The LR (sensitivity/1-specificity) tells you how much the odds of a disease will increase based on a positive result.
So, if you determine the pre-test probability to be 15% and the patient has an ulcer >2.0cm2 then the post-test probability would rise to 56%.
Remember:
Pre-test odds = pre-test probability /(1-pre-test probability)= 0.15/0.85=0.18 Post-test odds=pre-test odds * LR = 0.18 * 7.2 = 1.3
Post-test probability = post-test odds / (post test odds+1) = 1.3/2.3= 0.56 = 56%
or, more simply, use a Likelihood ratio nomogram
Similarly, a negative LR (1-sensitivity/specificity) tells you how much the odds of a disease decrease based on a negative test rest. So, for a patient whose pre-test probability is 15%, a normal MRI (ie a negative result), would change the post-test probability to 2.4%.
The article specifically noted that the studies that exist have not studied the significance of multiple findings in a patient. (As a personal commentary, I believe that it stands to reason that multiple positive findings would make a diagnosis of osteomyelitis more likely.)
Of note, there are no features of the medical history or other elements of the physical which were found to be helpful in the diagnosis, including presence of pain, fever or other systemic signs. Because it is established that diabetic ulcers tend to occur in patients with more advanced and poorly controlled diabetics, a history focusing on the diabetes history, including the presence of retinopathy, neuropathy, and nephropathy would be appropriate.
Reference: The Rational Clinical Examination: Does This Patient with Diabetes Have Osteomyelitis of the Lower Extremity?JAMA. 2008;299(7):806-13.

One comment on “The Rational Clinical Examination: Does This Patient with Diabetes Have Osteomyelitis of the Lower Extremity?”
The Pumpers: A New Paradigm in Diabetes Management
With some diabetic patients, insulin is necessary for their survival. As I recall, a man named Pauescu developed the concept of insulin replacement, and discovered the method of using insulin secreted from pigs as a replacement method for humans. Legend has it that this concept originated in a dream this man had on night several decades ago. Yet presently, this hormone which is naturally produced by the pancreas normally has advanced as far as treatment goes for the diabetic patient who is dependent on insulin for their treatment, and those are type 1 diabetic patients.
Recently, the Denver Bronco’s quarterback, Jay Cutler, was recently diagnosed with diabetes, a disease that affects over 20 million people. As I recall, part of his treatment regimen involves what is called an insulin pump. They are the size of a cell phone, approximately, and the users of such pumps are called, in the diabetic community, ‘pumpers’. Developed primarily for type 1, or insulin-dependent diabetic patients, the pumps can be used by some type 2 diabetic patients if they have some dependence on insulin replacement. The importance of the device is improved management of the disease, which can cause life-threatening consequences if the disease of diabetes is not controlled properly.
The three elements of an insulin pump include the pump itself and its components, such as the insulin tube for delivery of insulin, and a catheter that delivers basal and bolus doses, which are dependent on preset calculations. The amount of insulin is fast or rapid acting to ensure maximal pharmacokinetics to create intensive insulinotherapy for required diabetes management. These insulin amounts are ultimately determined by the patient’s doctor, who is usually an Endocrinologist, including bolus doses determined by the patients glucose level calculated with their carbohydrate intake, also known as the meal- time dose. Furthermore, the amount of insulin delivered by these methods is quite small due to the nature of the medication being rapid acting.
The makers of such pumps tend to partner with associations relevant to the disease of diabetes, as well as local chapters of such organizations as the ADA and Endocrinology societies that may exist, along with contacting diabetes educators frequently at different locations throughout the country. Unfortunately, there are few Endocrinologists in the United States, as it is not one of the more lucrative specialties of a doctor, so treatment of diabetes is dependent on many others who are not doctors, but patient care specialists regarding this disease.
Competing companies are few, as there are approximately 5 insulin pumps in the market, with Medtronic having the largest share of 30 percent, as I understand. Some pumps avoid the possibility of metabolic action therapy due to their dosing precision, in addition, there is at least one pump that has long acting lithium battery that averages about a 6 week lifespan, yet a pump user should have a battery replacement with them at all times. The personalized insulin and carbohydrate ratio provided by insulin pumps greatly reduces any incidence of such complications as hypoglycemia. Also, in addition to storing and recording glucose and carbohydrate values with a back up mechanisms, some insulin pumps have a low basal rate, which I understand is an advantage as well. Regardless, and in my opinion, the ultimate advantages of insulin pumps exist with all that are available to patients presently.
The cartridges of the insulin pumps hold a large number of units of insulin, which is an additional benefit. Further benefits include the fact that the pumps are convenient and reliable- especially if damage is avoided to the pump. Most importantly, the personal service provided to the patients by the caregivers of existing diabetic teams in health care facilities from hospitals to health care centers dedicated to the disease of diabetes ensures proper management of their disease, much to the benefit of those who have diabetes.
The market growth of insulin pumps is anticipated at over 10 percent a year, as only 20 percent of type 1 diabetic patients have utilized these pumps out of over a million type 1 diabetics in the United States. The market is speculated to be greater than one billion dollars and is expected to increase due to speculated growth of the Insulin pump market. Many believe this therapy is superior in comparison with previous treatment options available to diabetic patients, along with being less cumbersome for these patients. Because of this, there is decreased mortality along with increased quality of life for diabetics, as they are assured of better control of their disease in this rather convenient way. This has been proven by better A1C blood tests and glycemic control of diabetic patients.
The steady dosing maintains the patient’s metabolic requirements and decreases long term consequences associated with diabetics. It has also been proven that insulin pumps result in fewer hospitalizations, ER visits, and episodes of hypoglycemia due to the excellent control provided by the insulin pumps while providing the necessary intensive therapy for their disease state. The fast acting insulin used in these pumps is created through genetic engineering, I believe. In addition, patients are encouraged to check their blood sugar greater than three times a day while on the insulin pump. So this system is both friendly to the user and is clearly a very convenient form of treatment for them. The A1C test, by the way, is a blood test that reflects the diabetic patient’s average blood sugar over a period of a few months.
Those who may be interested in insulin pumps will include those described already, along with hospitals, long term care facilities, home health care agencies, pediatricians, and possibly dialysis clinics, to name a few. Most likely, those considered for insulin pumps will be diabetic patients that are unable to achieve compliance with their current treatment regimen, along with other benefits of insulin pumps stated so far.
The diabetes team for a diabetic patient may include an Endocrinologist, a diabetes educator, a dietician, along with the insulin pump representative. Follow ups with this team may include review the progress of the insulin pump for the patient and how the patient is tolerating the treatment. Often, classes can be scheduled through an institution or center regarding insulin pump training a few times a month. Education and training about the insulin pump may include the following:
1. Glycemic control importance and how to prevent and treat as needed
2. Basal and bolus concepts and how they contribute to the treatment
3. Pump basics and strategies. Negative effects stressed to pt. if their pump is not used properly.
4. Importance of knowing blood sugar and why. Definitions of terms like A1C
5. How to deliver a bolus dose after checking carbohydrate intake
6. How to check the pump’s memory
7. Troubleshooting, phone number access, and how to replace battery
8. Emphasize the safety of the insulin pump if operated correctly
9. Keeping a glucagon injection and spare battery with you
Ultimately after training others, it is important that the patient acknowledges understanding of how the device works, as well as the consequences that may occur if directions are not followed that are ultimately determined by the patients doctor. And fortunately, doctors and others who treat diabetes now have a new tool or device to assure compliance and longevity of these patients.
Innovation is a wonderful thing, such as what has been described. Control of such a large and devastating disease is of great importance, so there seems to be a much desired need for pumpers now and likely in the future.
Dan Abshear
Comments are closed.