Faculty Peer Reviewed
You have just completed a certification course in basic life support and are competent at performing cardiopulmonary resuscitation (CPR) using chest compressions, a CPR mask, a bag-valve mask with impedance threshold device, and an automated external defibrillator (AED), all interventions recommended by the American Heart Association (AHA) to improve circulation following a sudden cardiac arrest.[1] On your way home from the training center you see a man collapse and rush over to find him unresponsive, not breathing, and pulseless. You immediately initiate the “chain of survival†by ordering someone nearby to call 911 and someone else to search for an AED. You begin chest compressions, but fearing this man may have communicable diseases and a CPR mask or bag-valve mask is not available, you refrain from performing mouth-to-mouth ventilation. The emergency medical service (EMS) personnel arrive 5 minutes later and take over the resuscitation effort. The scene clears and you wonder: how much did my actions help this man’s chances of survival? Did failure to deliver rescue breaths hurt these chances?
Each year over 300,000 Americans suffer an out-of-hospital cardiac arrest (OHCA), defined as a cessation of cardiac mechanical activity that occurs outside of the hospital and is confirmed by the absence of circulation signs.[2,3] Though an OHCA can occur from noncardiac causes such as trauma or drowning, the majority of such events have a primary cardiac cause and a poor 6.5% overall survival rate to hospital discharge.[2] For most of these victims the scenario described above is the best they can realistically hope for, as only 8.6% of OHCAs are witnessed by EMS.[4] In the remaining cases, initiation of the chain of survival depends on family members or strangers while the victim’s chances of survival falls 7-10% every minute without bystander CPR until defibrillation.[2] Considering that the median time delay between calling 911 and EMS arrival is 5.3 minutes,[4,5] it is vital that bystanders perform CPR as soon as possible.
Even when bystanders witness an OHCA, studies show that they perform CPR in the minority of cases. According to the Center for Disease Control and Prevention (CDC) surveillance data on victims of OHCA of presumed cardiac cause who received CPR in the prehospital setting between 2005 and 2010,[6] the overall survival rate to hospital discharge was 9.6%. Although 37.6% of OHCA events were witnessed by bystanders, only 43.8% of them performed CPR and increased survival rate to 11.2% compared with 7.0% in victims who did not receive CPR prior to EMS arrival (p<0.001). In other words, the CDC’s analysis showed bystander CPR to have a 37.5% relative risk reduction and a number needed to treat of 24. To put this effect into perspective, aspirin given to prevent major cardiovascular events has a number needed to treat of 253 in patients without clinical evidence of cardiovascular disease.[7]
Research indicates that the infrequent performance of bystander CPR is due, in large part, to a reluctance to perform mouth-to-mouth ventilation. In a 1995 survey, only 15% of 975 respondents reported a willingness to perform chest compressions with mouth-to-mouth ventilation on a stranger, whereas 68% responded that they would “definitely†perform chest compressions alone if it were offered as an effective alternate CPR technique.[8] Since then, many studies have examined survival rates between conventional CPR, which includes rescue breathing, and compression-only CPR, and concluded that omitting ventilations from the bystander sequence confers no negative impact.[1, 9-11] As a result, the AHA Guidelines now recommend that “laypersons should be encouraged to do compression-only CPR if they are unable or unwilling to provide rescue breaths†on the basis that provision of compression-only CPR is superior to no CPR.[7,9]
Lastly, it should be noted that in addition to bystander CPR, several other parameters have been identified as significant predictors of OHCA survival. They include the location of the cardiac arrest, the presenting arrest rhythm, who first applied the AED, and whether there was a return of spontaneous circulation (ROSC) in the field.[4-6,12] The CDC reported that 84.1% of OHCAs occurred in the home and had a survival rate of 7.0%, whereas OHCAs that occurred in public had a survival rate of 20.2%. Of the bystander-witnessed OHCAs, an AED was applied prior to EMS arrival in 3.7% of cases, wherein survival rate was 23.5%. If the victim was found in a shockable arrest rhythm, survival rate was 27.1%, and if ROSC on the field was achieved, survival rate was 26.3%. Although understanding the reasons for these varying OHCA survival rates is important, and is explored extensively in the literature,[6,12] it is beyond the scope of this discussion.
From a young age we hear the mantra, “CPR saves lives.†We see CPR instructional posters on the walls of eating establishments and resuscitation efforts in action movies and TV shows. Although the prognosis of OHCAs remains poor, bystander CPR has been found to contribute a 4.2% overall increase in survival to hospital discharge compared with calling 911 alone. However, studies show that only a minority of bystanders perform CPR, discouraged by the thought of performing mouth-to-mouth ventilations on a stranger. Perhaps if these onlookers had known that compression-only CPR may be as effective as conventional CPR, many lives could have been saved. Now that compression-only CPR is recommended by the AHA guidelines, hopefully more bystanders will embrace the opportunity to help an OHCA victim’s chances of survival.
Andrew L. Weinstein is a 3rd year medical student at NYU School of Medicine
Peer reviewed by Dr. Kevin Felner, MD, Pulmonary, Critical Care, NYU Langone Medical Center
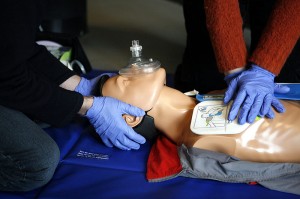
Image courtesy of Wikimedia Commons
References
1. Field JM, Hazinski MF, Sayre MR, et al. Part 1: executive summary: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation. 2010;122(18 Suppl 3):S640-656. http://circ.ahajournals.org/content/122/18_suppl_3/S640.long
2. Roger VL, Go AS, Lloyd-Jones DM, et al. Heart disease and stroke statistics–2011 update: a report from the American Heart Association. Circulation. 2011;123(4):e18–e209. http://circ.ahajournals.org/content/123/4/e18.long
3. Jacobs I, Nadkarni V, Bahr J, et al. Cardiac arrest and cardiopulmonary resuscitation outcome reports: update and simplification of the Utstein templates for resuscitation registries: a statement for healthcare professionals from a task force of the International Liaison Committee on Resuscitation (American Heart Association, European Resuscitation Council, Australian Resuscitation Council, New Zealand Resuscitation Council, Heart and Stroke Foundation of Canada, InterAmerican Heart Foundation, Resuscitation Councils of Southern Africa). Circulation. 2004;110(21):3385–3397. http://circ.ahajournals.org/content/110/21/3385.long
4. Weisfeldt ML, Everson-Steward S, Sitlani C, et al. Ventricular tachyarrhythmias after cardiac arrest in public versus at home. N Engl J Med. 2011;364:313-21. http://www.nejm.org/doi/full/10.1056/NEJMoa1010663
5. Weisfeldt ML, Sitlani CM, Ornato JP, et al. Survival after application of automatic external defibrillators before arrival of the emergency medical system: evaluation in the resuscitation outcomes consortium population of 21 million. J Am Coll Cardiol. 2010;55:1713-1720. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3008654/?tool=pubmed
6. McNally B, Robb R, Mehta M, et al. Out-of-hospital cardiac arrest surveillance – cardiac arrest registry to enhance survival, United States, October 1, 2005 – December 31, 2005. MMWR. 2011;60(SS08);1-19. http://www.cdc.gov/mmwr/preview/mmwrhtml/ss6008a1.htm
7. Berger JS, Lala A, Krantz MJ, Baker GS, Hiatt WR. Aspirin for the prevention of cardiovascular events in patients without clinical cardiovascular disease: A meta-analysis of randomized trials. Am Heart J. 2011;162(1):115-124.e2. http://www.ahjonline.com/article/S0002-8703(11)00272-9/fulltext
8. Locke CJ, Berg RA, Sanders AB, et al. Bystander cardiopulmonary resuscitation: concerns about mouth-to-mouth contact. Arch Intern Med. 1995;155:938–43.
9. Sayre MR, Berg RA, Cave DM, Page RL, Potts J, White RD; American Heart Association Emergency Cardiovascular Care Committee. Hands-only (compression-only) cardiopulmonary resuscitation: a call to action for bystander response to adults who experience out-of-hospital sudden cardiac arrest: a science advisory for the public from the American Heart Association Emergency Cardiovascular Care Committee. Circulation. 2008;117(16):2162-7. http://circ.ahajournals.org/content/117/16/2162.long
10. Hallstrom A, Cobb L, Johnson E, Copass M. Cardiopulmonary resuscitation by chest compression alone or with mouth-to-mouth ventilation. N Engl J Med. 2000;342:1546-1553. http://www.nejm.org/doi/full/10.1056/NEJM200005253422101
11. Rea TD, Fahrenbruch C, Culley L, et al. CPR with chest compressions alone or with rescue breathing. N Engl J Med. 2010;363:423-33. http://www.nejm.org/doi/full/10.1056/NEJMoa0908993
12. Sasson C, Rogers MAM, Dahl J, Kellermann AL. Predictors of survival from out-of-hospital cardiac arrest: a systematic review and meta-analysis. Circ Cardiovasc Qual Outcomes. 2010;3:63-81. http://circoutcomes.ahajournals.org/content/3/1/63.long

One comment on “Bystander CPR: How Much Does It Help?”
Comments are closed.