Peer Reviewed
As of mid-August 2012, the CDC had reported 1118 cases of West Nile virus (WNV) infections and 41 related deaths, which, pro rata, made 2012 the most prolific year for WNV in the United States [1]. Although West Nile’s classification as a public health crisis remains debatable, the lack of treatment and vaccination options make associated severe infections a real threat.
West Nile virus, a single-stranded RNA virus of the Flavivirus family, was first isolated in Uganda in 1937 [2]. Since its emergence in the United States in 1999, there have been approximately 33,000 cases and 1,200 deaths. The virus is maintained in an enzootic cycle between over 300 avian species and Culex mosquitos, which act as the transmission vector. It is believed that only birds can maintain high enough viral loads to be infectious hosts, as humans and other mammals result in “dead-end†infections [2].
Upon viral inoculation via an infected mosquito, WNV initially infects local dendritic cells in the skin, followed by viral amplification in regional lymph nodes. Subsequently, a mild viremia, which is cleared in approximately 1 week by a rapid IgM response, results in a multi-organ infection as well as highly variable systemic symptoms [2]. Only 20-40% of individuals who are infected will become symptomatic after the virus’s 2-14 day incubation period. The majority of these individuals develop a mild, flu-like, self-limiting illness known as West Nile fever [3].
Less than 1% of infected patients, however, will develop severe neuroinvasive disease. The manifestations of these severe infections include meningitis, encephalitis, and acute flaccid paralysis. WNV infection of the central nervous system can be definitively diagnosed by the presence of West Nile IgM in the cerebrospinal fluid, detectable in greater than 90% of patients with neuroinvasive disease by day 8 of presentation [4]. Of clinical significance, serum WNV IgM false-positives are possible with recent yellow fever or Japanese encephalitis vaccination or a recent infection with a Flavivirus (St. Louis encephalitis or dengue). Supplemental testing with plaque-reduction neutralization testing and nucleic acid amplification testing can increase the specificity and accuracy, respectively, of serum IgM detection [4].
In neuroinvasive disease, viral entry into the CNS is likely mediated by both an increase in blood-brain barrier permeability, secondary to local TNF-alpha production, and by retrograde transmission via peripheral neurons [2]. West Nile meningitis, which represents 40% of West Nile neuroinvasive disease, is associated with a favorable prognosis with <1% mortality [5]. Approximately 50% of neuroinvasive infections, especially in the elderly and immunocompromised, are characterized as West Nile encephalitis. These infections result in a 20% in-hospital mortality rate as well as persistent Parkinsonian symptoms in up to 40% of survivors [5]. Finally, the most devastating disease variant is West Nile acute flaccid paralysis (WNP), which accounts for approximately 10% of neuroinvasive disease [5]. Interestingly, WNP is not a transient demyelinating process, as seen with infection-mediated Guillain-Barré syndrome; rather, the paralysis is due to irreversible anterior horn neuronal damage consistent with poliomyelitis [3]. The extent of paralysis can range form monoplegia to quadriplegia with neuromuscular respiratory failure, which results in mortality rates ranging from 10-50% [5]. In addition to short-term morbidity and mortality, neuroinvasive West Nile disease is associated with persistent fatigue, weakness, ataxia, and cognitive dysfunction in nearly 50% of survivors in long-term follow-up studies [5].
Although the probability of severe disease is <1% of the relatively small number of total West Nile infections, there is currently no specific approved therapy for WNV. Therapeutic candidates for WNV such as ribavirin, mycophenolic acid, and interferon-alpha have demonstrated efficacy in vitro, but they have failed to show a clinical benefit [6]. Passive immunity with anti-WNV antibodies has demonstrated reduction in mortality in animal models as well as improvement in neuroinvasive disease in small human trials, particularly among elderly and immunocompromised patients who have high viral titers [6]. This promising therapeutic option is currently undergoing phase 2 clinical trials. Another experimental treatment approach involves small-interfering RNA (siRNA) to target intracellular viral RNA, thus limiting viral translation and subsequent replication. While this form of treatment is efficacious in early-diagnosed infections, advances in the delivery system technology for siRNA will be a required next step before widespread clinical use [6].
Until the establishment of a WNV vaccine or effective treatment, the single most important (and least expensive) intervention is prevention, which is particularly important in the peak months of July through September [4]. The CDC recommends DEET-based insect repellents and mosquito nets for personal protection, especially at night and near sources of still water. At the community level, some areas are adopting strategically timed low-volume insecticide applications, which appear to effectively decrease WNV transmission [4]. The CDC also uses local authorities to track bird deaths in order to assess for avian WNV infections, thus better identifying high-risk locations [7].
While WNV may present as an incurable neuroinvasive disease (as is often portrayed by the media), statistically speaking, over 99% of infections range from asymptomatic to a self-limiting flu-like illness, especially in immunocompetent individuals. Regardless of the favorable probabilities, appropriate precautions and continued antiviral research will hopefully soon eliminate 100% of this annual viral threat.
Julian Horwitz is a 4th year medical student at NYU School of Medicine
Peer Reviewed by Harold Horowitz, MD, Medicine,  NYU Langone Medical Center
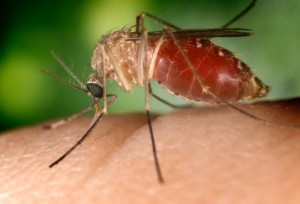
Image courtesy of Wikimedia Commons
References:
[1] Kaiser J. Public health. Outbreak pattern stymies vaccine work. Science. 2012:337(6098):1030. http://www.sciencemag.org/content/337/6098/1030.short
[2] Ulbert S. West Nile virus: the complex biology of an emerging pathogen. Intervirology. 2011:54(4):171-184. http://www.ncbi.nlm.nih.gov/pubmed/21576931
[3] Kramer LD, Li J, Shi PY. West Nile virus. Lancet Neurol. 2007:6(2):171-181. http://www.ncbi.nlm.nih.gov/pubmed/17239804
[4] Peterson LR, Brault AC, Nasci RS. West Nile virus: review of the literature. JAMA. 2013:310(3):308-315. http://www.ncbi.nlm.nih.gov/pubmed/23860989
[5] Sejvar JJ. The long-term outcomes of human West Nile virus infection. Clin Infect Dis. 2007:44(12):1617-1624.  http://cid.oxfordjournals.org/content/44/12/1617.full
[6] Diamond MS. Progress on the development of therapeutics against West Nile virus. Antiviral Res. 2009:83(3):214-227. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2759769/
[7] Centers for Disease Control and Prevention. Epidemic/epizootic West Nile virus in the United States: guidelines for surveillance, prevention, and control. http://www.cdc.gov/westnile/resources/pdfs/wnvguidelines.pdf. Â Revised June 14, 2013. Accessed February 19, 2014.