Vivian Hayashi MD, Robert Smith MD
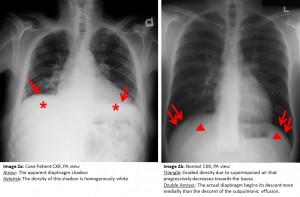
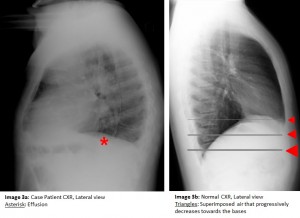
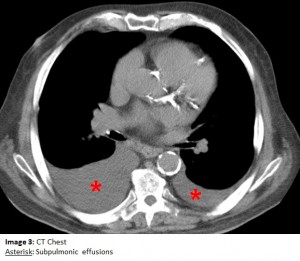
The answer to the mystery quiz is pleural effusions, specifically, bilateral subpulmonic effusions. The chest radiograph shows a number of findings: (1) the apparent diaphragm shadow is in fact fluid sandwiched between the undersurface of the lung and the actual diaphragm (Image 2a, arrow); (2) the density of this shadow is homogenously white (Image 2a, asterisk) and differs from a normal diaphragm which has a graded density (Image 2b, triangle) due to superimposed air that progressively decreases towards the bases (Image 3b); (3) the actual diaphragm (Image 2b, double arrows) begins its descent more medially than the descent of the subpulmonic effusion (Image 2a); and (4) the distance between the top of the gas bubble and the left hemidiaphragm is very small in the normal radiograph (Image 2b), compared with the increased distance due to the subpulmonic effusion (Image 2a). The chest CT confirms that the findings on the standard radiograph represent subpulmonic effusions (Image 4, asterisk).
Subpulmonic effusions, a subcategory of pleural effusions, are likely due to localized pressure gradients within the pleural space and possible unrecognized, subclinical adhesions. The most common appearance of a moderately sized pleural effusion shows a meniscus, unlike the downsloping lateral edge of a subpulmonic effusion. Another means to confirm that a subpulmonic effusion is present would be a lateral decubitus film that shows the subpulmonic fluid layering laterally along the chest wall. Moreover, simple ultrasonography can also confirm the presence of pleural fluid. There is no particular significance attributable to subpulmonic effusions other than recognizing that pleural fluid is indeed present. They are evaluated and managed no differently than standard pleural effusions.

One comment on “Mystery Quiz-The Answer”
Interesting. Adhesions are more likely to be the cause but subpulmonic effusions are still mysterious.
Comments are closed.