Peer Reviewed
You are a third-year internal medicine resident finishing your night shift at John Doe Hospital. Your shift so far was challenging to say the least: six admissions to the general medicine service. It was a hodgepodge of elderly patients with multiple medical co-morbidities sprinkled with difficult family members. Throw in two rapid responses (led by none-other than yourself) for altered mental status and hypoxia for good measure. As you lay yourself down on the hard, 1980’s-era sofa in the medicine call room, the last words you want to hear are blasted over the hospital speakers, “code 4000 17-north.†You jump off the sofa, hurriedly grab your stethoscope and an ACLS pocket guide and speed walk to the 17-north medicine unit. On arrival, you find Mr. Smith, the elderly gentleman you admitted earlier with likely bacterial pneumonia who cracked a joke about how young you look to be a physician lying unconscious in his hospital bed with the nurse compressing his chest in a rhythmic fashion. You confirm that Mr. Smith is full code, identify the rhythm as PEA (Pulseless Electrical Activity), instruct a nurse to administer 1mg of intravenous epinephrine, and command the newly minted intern to operate the bag mask at the head of the bed. Out of the corner of your eye you see the anesthesia resident swoop inside the room, intubation kit in hand. Within three minutes, Mr. Smith is successfully intubated. You instruct James, one of your favorite and most trustworthy nurses, to “please attach the end tidal CO2 to the ET tube and cardiac monitor.†To your pleasant surprise, the monitor shows an EtCO2 level of 14 mmHg. After one minute, the EtCO2 level jumps up to 40 mmHg, ROSC (return of spontaneous circulation) is obtained, and Mr. Smith is transferred to the medical ICU. As you sit down and reflect on this case, you begin to wonder about the evidence supporting end tidal CO2 use.
End tidal CO2, or waveform capnography, is one of the most novel innovations in cardiopulmonary resuscitation (CPR) in the past 20 to 30 years. In the 1970’s and 80’s, studies in animal models elucidated the physiology and potential utility of end tidal CO2 monitoring. Grundler et al. in Circulation demonstrated that during the initial period of CPR, venous acidemia and simultaneous arterial alkalemia caused a significant increase in mixed carbon dioxide tension. This increase was closely related to a reduction in both the partial pressure (EtCO2) and the volume of expired CO2 [1]. Later, Weil et al. demonstrated via thermodilution technique that EtCO2 levels positively correlate with cardiac output during CPR and therefore can be used as a noninvasive measure of cardiac output [2]. In a landmark study published in The New England Journal of Medicine in 1988, Falk et al. demonstrated this same principal in humans [3]. In this single-center study, Falk et al. prospectively analyzed 13 cardiac arrests in ten ICU patients. All patients had endotracheal tubes in place and EtCO2 was measured using an infrared absorption carbon dioxide monitor. The authors found that with the onset of cardiac arrest, there was a decrease in the EtCO2 over a period of one minute, to 0.4 ± 0.4 percent. After the initiation of chest compressions, the EtCO2 increased within 30 seconds to 1.0 ± 0.5 percent. Finally, with the return of spontaneous circulation, the EtCO2 increased within 30 seconds from 1.3 ± 0.5 percent to an overshoot value of 3.7 ± 2.1 percent. The authors verified in humans what was seen in animal models that there was a direct correlation between end-tidal carbon dioxide concentration and cardiac output produced by precordial compressions. This study helped put end-tidal CO2 on the map.
After this landmark study was published, numerous studies further demonstrated that EtCO2 varies directly with the cardiac output produced by chest compressions [4,5]. As such, EtCO2 provides the healthcare worker with an instantaneous measure of efficacy of chest compressions being performed. In fact, the latest AHA guidelines for ACLS (advanced cardiac life support) recommend maintaining an EtCO2 level of at least 10-22 mmHg, which represents high quality chest compressions [6].
Beyond chest compression efficacy, waveform capnography has several other applications during CPR. Interestingly, EtCO2 level has been shown to be a prognostic indicator in cardiac arrest patients. Grmec et al prospectively studied EtCO2 levels during CPR in 139 out-of-hospital cardiac arrest patients. This study had two significant findings. First, the initial, average, and final EtCO2 values were significantly higher in resuscitated patients as compared to non-resuscitated patients. Second, none of the patients with initial, average, or final EtCO2 values less than 10 mmHg were successfully resuscitated [7]. This study emphasizes the importance of effective chest compressions to maintain an EtCO2 level of at least 10-22 mmHg, as stated earlier.
Fascinatingly, EtCO2 is the earliest indicator of the return of spontaneous circulation [3,4,8]. This sudden rise in EtCO2 occurs as the patient’s cardiac output rapidly increases and the CO2 that has accumulated during cardiac arrest is carried to the lungs and exhaled. It should also be noted that once this sudden rise in EtCO2 is seen, chest compressions can be safely stopped as this rise necessitates (and therefore indicates) the establishment of a perfusing rhythm [9].
Together, waveform capnography has dramatically enhanced our abilities to perform safe and effective CPR. This measure is able to inform the healthcare provider whether he/she is performing adequate chest compressions, whether the patient has a good prognosis of survival, and when ROSC has been obtained. It is for these reasons that waveform capnography be utilized during all cardiac arrests.
Dr. David Pineles is a internal medicine resident at NYU Langone Health
Peer reviewed by Nishay Chitkara, MD, Assistant Professor of Medicine (Clinical), Internal Medicine, Division of Pulmonary, Critical Care, and Sleep Medicine, NYU Langone Health
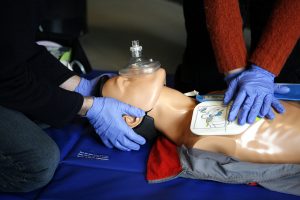
Image courtesy of Wikimedia Commons
Reference:
1. Grundler W, Weil MH, Rackow EC. Arteriovenous carbon dioxide and pH gradients during cardiac arrest. Circulation. 1986;74(5):1071-4.  https://www.ncbi.nlm.nih.gov/pubmed/3094980
2. Weil MH, Bisera J, Trevino RP, Rackow EC. Cardiac output and end-tidal carbon dioxide. Crit Care Med. 1985;13(11):907-9.
3. Falk JL, Rackow EC, Weil MH. End-tidal carbon dioxide concentration during cardiopulmonary resuscitation. N Engl J Med. 1988;318(10):607-11.  https://www.ncbi.nlm.nih.gov/pubmed/3125432
4. Garnett AR, Ornato JP, Gonzalez ER, Johnson EB. End-tidal carbon dioxide monitoring during cardiopulmonary resuscitation. JAMA. 1987;257(4):512-5.
5. Ornato JP, Levine RL, Young DS, Racht EM, Garnett AR, Gonzalez ER. The effect of applied chest compression force on systemic arterial pressure and end-tidal carbon dioxide concentration during CPR in human beings. Ann Emerg Med. 1989;18(7):732-7.  https://www.ncbi.nlm.nih.gov/pubmed/2500044
6. Quantitative waveform capnography. https://acls-algorithms.com/waveform-capnography/
7. Grmec S, Klemen P. Does the end-tidal carbon dioxide (EtCO2) concentration have prognostic value during out-of-hospital cardiac arrest?. Eur J Emerg Med. 2001;8(4):263-9.  https://www.ncbi.nlm.nih.gov/pubmed/11785591
8. Pokorná M, Necas E, KratochvÃl J, Skripský R, AndrlÃk M, Franek O. A sudden increase in partial pressure end-tidal carbon dioxide (P(ET)CO(2)) at the moment of return of spontaneous circulation. J Emerg Med. 2010;38(5):614-21.  https://www.ncbi.nlm.nih.gov/pubmed/19570645
9. Neumar RW, Otto CW, Link MS, et al. Part 8: adult advanced cardiovascular life support: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010; 122:S729.  https://www.ncbi.nlm.nih.gov/pubmed/20956224
Commentary by Nishay Chitkara, MD
The author’s excellent discussion highlights the essential role that EtCO2 monitoring can play in CPR. Indeed, EtCO2 measurements indirectly reflect pulmonary blood flow / alveolar ventilation and cardiac output, in the relatively low-flow state generated by chest compressions. During the combined state of low-flow and fixed minute ventilation that characterizes CPR, EtCO2 is primarily determined by pulmonary blood flow, and low EtCO2 values can indicate insufficient cardiac output. However, it is also important to consider other causes of low EtCO2 values, some of which may result from underlying conditions that are contributory to cardiac arrest: bronchospasm, mucous plugging of the ETT, kinking of the ETT, alveolar fluid in the ETT, hyperventilation, or an airway with a an air leak. In non-intubated patients, EtCO2 measurement may not be as consistent or reliable a tool as it is for intubated patients.
As stated, quantitative waveform capnography can be an excellent indicator of high quality CPR when an EtCO2 >10 mm Hg is targeted. A sudden and sustained increase in EtCO2 to >40 mm Hg can confirm return of spontaneous circulation (ROSC) in the patient who has regained a pulse and blood pressure following CPR. It indicates a cardiac output adequate to restore pulmonary blood flow.
EtCO2 measurement (absent any confounding factors) can also be used in the context of other clinical data to decide upon appropriate timing of cessation of resuscitative efforts. Some data suggest that failure to achieve an EtCO2 >10 mm Hg, despite optimal resuscitation for 20 minutes, may be associated with a low likelihood of ROSC.
References:
1. Part 7: Adult Advanced Cardiovascular Life Support: 2015 American Heart Association Guidelines Update for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care
Link MS, Berkow LC, Kudenchuk PJ, Halperin HR, Hess EP, Moitra VK, Neumar RW, O’Neil BJ, Paxton JH, Silvers SM, White RD, Yannopoulos D, Donnino MW.
Circulation. 2015 Nov 3;132(18 Suppl 2):S444-64. doi: 10.1161/CIR.0000000000000261.
2. Systematic Review and Meta-Analysis of End-Tidal Carbon Dioxide Values Associated With Return of Spontaneous Circulation During Cardiopulmonary Resuscitation
Hartmann SM, Farris RW, Di Gennaro JL, Roberts JS.
J Intensive Care Med. 2015 Oct;30(7):426-35. doi: 10.1177/0885066614530839. Epub 2014 Apr 22.