Peer Reviewed
During my trip to India, the “family bonding†reached a new level when I shared my upper respiratory infection with my parents and sister. On day two of my father’s rhinorrhea and cough, a family friend, who is a doctor, suggested he take antibiotics for a few days. There were extra in the house, or he could buy erythromycin tablets for only 35 rupees (less than $1) in the shop down the street without a prescription. I was shocked. Not only was it unbelievably easy to buy antibiotics, but people were also using these medications for the slightest of ailments. While other factors also play a role, it started to make sense why India has one of the highest rates of antimicrobial resistance [1]. Nevertheless, antimicrobial resistance is a danger that threatens all of us, across the globe [2].
In order to comprehend why the threat of antimicrobial resistance is growing, it is important to understand the changing paradigm of antibiotic research. The first well known antibiotic was Salvarsan, a drug discovered in the early 1900s to treat syphilis. This drug, along with many of the other earliest antibiotics, was discovered through a large-scale, systematic screening approach, in which hundreds of compounds were synthesized and tested against a drug target, such as an animal infected with a specific microbe or agar-medium plated with bacteria [3,4]. The next major antibiotics were Prontosil, a sulfanilamide, which was introduced in 1937, and penicillin, which was discovered by Alexander Fleming in 1928 and introduced in 1943 [3,5,6]. This was followed by the identifications of streptomycin and para-amino salicylic acid (PAS) for the treatment of tuberculosis in 1944 [7,8]. With this approach to drug discovery, the development of new antibiotic classes flourished in the 1950s to 1970s as tetracyclines, macrolides, aminoglycosides, and quinolones were introduced [9].
Since then, discovery of novel antibiotics has significantly declined. Not only are there fewer antibiotics being developed overall, but also the approach to new drugs has focused on the modification of preexisting drugs rather than discovery of new classes. Thus, there is a high chance that, similar to the preexisting drugs in these classes, bacteria will acquire resistance to the newer antibiotics as well [3,10].
Resistance to antimicrobials has its own similarly longstanding history, with resistance to penicillin identified in 1940 and resistance to other antibiotics arising in the years after, largely due to the overuse of antibiotics. A study analyzing antibiotic use in ambulatory care settings in the US estimated that 30% of antibiotics were inappropriately prescribed [11]. Antibiotics are often prescribed for longer courses than recommended, which can lead to antimicrobial resistance, with the durations of greater than two-thirds of antibiotics courses for respiratory indications exceeding recommended guidelines [12–15]. Moreover, studies have shown a strong temporal correlation between antibiotic use and antibiotic resistance [16]. Inappropriate prescriptions and non-compliance with antibiotic therapy, as well as agricultural use of antibiotics, have acted as a catalyst for this process by creating environmental reservoirs for antimicrobial resistance to develop [10,17]. As a result, many bacteria responsible for both community-acquired and nosocomial infections have developed multi-drug resistance, increasing morbidity and mortality from these pathogens [17,18]. For example, between 1997 and 2018, the rate of Streptococcus pneumoniae resistance to erythromycin increased from 14.9% to 28.8%. Between 2006 and 2018, the rate of group A Streptococcus resistance to clindamycin increased from 1.7% to 24.2% [19]. According to a CDC report on antibiotic resistance, in the United States alone, more than 35,000 people die each year as a result of antibiotic-resistant pathogens [20].
If the threat of antimicrobial resistance is continuing to grow, why has the development of novel antibiotics continued to remain low? The answer largely boils down to economics. The cost of developing novel antibiotics, conducting clinical trials, and overcoming regulatory barriers is high [9,21]. Moreover, antibiotics are not as profitable as other drugs [21]. Some physicians may restrain from prescribing new antibiotics, reserving them for last-line treatments or for severe infections in the hopes of limiting bacterial resistance to that agent [22]. Even with this restrained prescribing, there is a high chance that resistance to that agent will inevitably develop down the line, further decreasing its economic potential. In addition, antibiotics are typically prescribed in low quantities for a short duration, unlike drugs such as metformin or statins that are used to manage chronic diseases [21]. Given the recent success of antiviral agents in treating highly prevalent diseases, such as sofosbuvir/ledipsavir for Hepatitis C and antiretroviral therapies for HIV, many pharmaceutical companies have also become more interested in investing in antivirals [23,24]. Thus, many major pharmaceutical companies have shifted their focus away from antibiotic research and towards more profitable markets, resulting in the dwindling of antibiotic development [9,21].
Amidst the current antibiotic research paradigm, new approaches to treating infections are being investigated. For example, vaccines and antibodies against pathogens such as Staphylococcus aureus and Clostridium difficile are being investigated. In phase 1 and 2 trials, a C. difficile toxoid vaccine was shown to be safe and effective in inducing antibodies that neutralize and bind to toxins A and B. The vaccine is currently undergoing phase 3 trials with the aim of eventually administering the toxoid to patients prior to planned inpatient procedures or antibiotic courses to prevent infection in those with underlying medical conditions [25]. Vaccines for S. auerus have shown less potential; however, a human monoclonal antibody that binds Protein A and allows for phagocytosis of the pathogen has been identified. A study found that the survival rate of mice infected with a high load of MRSA was significantly higher in those treated with both vancomycin and the antibody compared to vancomycin alone. This suggests a potential for co-therapy for patients with severe S. auerus infections [26].
Another approach has been the use of bacteriophages for lysis of bacteria, particularly those that are foodborne or biofilm-producing such as Listeria monocytogenes, Salmonella, and Pseudomonas aeruginosa. Several bacteriophages have been FDA-approved for use in the food industry and there is ongoing research on expanding the applications of these agents for therapeutic use. For example, in a study on the therapeutic potential of bacteriophages against multi-drug resistant pneumonia, a novel chimeric phage lysine was shown to increase protection against Streptococcus pneumonia in a mouse bacteremia model [27].
Additional antibiotic alternatives include antimicrobial peptides, which disrupt bacterial cell walls and probiotics, which can alter the gut microbial flora such that it can overcome pathogenic bacteria [18]. Many of these approaches are in the early stages of investigation and have many challenges to overcome before being introduced for therapeutic human use. Moreover, similar to other drugs, these novel agents come with limitations such as toxicities and cost of production. Nevertheless, the investment of pharmaceutical companies in this research and the innovativeness provide hope that the threat of antimicrobial resistance may be attenuated [18,28].
While these novel agents continue to be developed, as clinicians we must do our part in addressing antimicrobial resistance. This may involve educating patients on the importance of completing their course of antibiotics, explaining indications for antibiotics, prescribing the shortest course recommended, and not overprescribing medications [18,29]. However, there is a need for further exploration of attitudes towards antibiotics in order for such education to be effective. A WHO survey showed, for example, that a majority of people in Russia, China, and India believe it is okay to share antibiotics with family and friends. The challenges posed by these beliefs are further amplified by the ability to self-prescribe antibiotics in countries such as India. Thus, additional insight into the beliefs of these populations is necessary in order to provide culturally tailored education to patients and further strengthen our campaign against antimicrobial resistance [29].
Avani Kolla is a medical student in the NYU Grossman School of Medicine
Commentary by Melanie Maslow, MD, FACP, FIDSA
This excellent article highlights the multiple interrelated factors leading to the global public health threat posed by the increasing frequency of multidrug-resistant (MDR) pathogens worldwide. The Infectious Diseases Society of America (IDSA) has been vocal for almost two decades in addressing the need for development of new classes of antibiotics to treat MDR pathogens. In 2010, the IDSA began the “10 x ’20 Initiativeâ€, endorsing the development and FDA approval of 10 “novel, efficacious, and safe systemically administered antibacterial agents†[1]. Of the antibiotics approved by 2020, the majority are modifications of prior classes that improve the spectrum of activity and overcome resistance. They include five new beta-lactam-beta-lactamase combinations, two new tetracycline antibiotics and a new fluoroquinolone. Older antibiotics that were sidelined such as sulopenem (a carbapenem), plazomicin (an aminoglycoside) and intravenous fosfomycin are undergoing a reassessment. The two novel agents are cefiderocol, a siderophore cephalosporin, and lefamulin, a pleuromutilin, a new class of protein synthetic inhibitors [2–4]. Cefiderocol has activity against some carbapenem-resistant MDR gram-negative bacteria whereas lefamulin is in studies as an alternative for treatment of community-acquired pneumonia.
Why has the development of novel antimicrobials slowed? One proposed reason is that pharmaceutical companies have prioritized funding to medications for chronic medical illnesses that generate a larger financial gain. The invention of new antimicrobials is difficult, time-consuming and subject to strict regulatory approval. Until novel antimicrobials become available, we must continue to educate providers about the dangers of overprescribing antibiotics, shorten courses to adhere to guidelines and continue aggressive antimicrobial stewardship programs.
Dr. Melanie Maslow is a professor in the Department of Medicine (Division of Infectious Diseases)
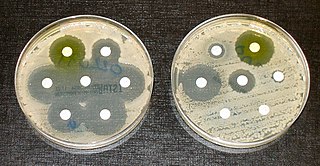
Image courtesy Wikimedia Commons
References
- Taneja N, Sharma M. Antimicrobial resistance in the environment: The Indian scenario. The Indian journal of medical research. 2019;149(2):119-128. https://pubmed.ncbi.nlm.nih.gov/31219076/
- Organization WH. Lack of new antibiotics threatens global efforts to contain drug-resistant infections. https://www.who.int/news-room/detail/17-01-2020-lack-of-new-antibiotics-threatens-global-efforts-to-contain-drug-resistant-infections. Published 2020. Accessed. https://www.who.int/news-room/detail/17-01-2020-lack-of-new-antibiotics-threatens-global-efforts-to-contain-drug-resistant-infections
- Aminov RI. A brief history of the antibiotic era: lessons learned and challenges for the future. Frontiers in microbiology. 2010;1:134. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3109405/
- Hughes JP, Rees S, Kalindjian SB, Philpott KL. Principles of early drug discovery. British journal of pharmacology. 2011;162(6):1239-1249. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3058157/
- Fleming A. On the Antibacterial Action of Cultures of a Penicillium, with Special Reference to their Use in the Isolation of B. influenzæ. Br J Exp Pathol. 1929;10(3):226-236. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2048009/
- Mahoney J. AR, Harris A. Penicillin Treatment of Early Syphilis—a Preliminary Report. Verer Dis Inform. 1943;24:355–357. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1527687/
- Iseman MD. Tuberculosis therapy: past, present and future. European Respiratory Journal. 2002;20(36 suppl):87S. http://erj.ersjournals.com/content/20/36_suppl/87S.abstract
- Council MR. Treatment of Pulmonary Tuberculosis with Streptomycin and Para-Amino-Salicylic Acid. Quality & safety in health care. 1950;2. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2039351/
- Ventola CL. The antibiotic resistance crisis: part 1: causes and threats. P & T : a peer-reviewed journal for formulary management. 2015;40(4):277-283. https://pubmed.ncbi.nlm.nih.gov/25859123/
- Lobanovska M, Pilla G. Penicillin’s Discovery and Antibiotic Resistance: Lessons for the Future? The Yale journal of biology and medicine. 2017;90(1):135-145. https://pubmed.ncbi.nlm.nih.gov/28356901/
- Fleming-Dutra KE, Hersh AL, Shapiro DJ, et al. Prevalence of Inappropriate Antibiotic Prescriptions Among US Ambulatory Care Visits, 2010-2011. Jama. 2016;315(17):1864-1873. https://jamanetwork.com/journals/jama/fullarticle/2518263
- King LM, Sanchez GV, Bartoces M, Hicks LA, Fleming-Dutra KE. Antibiotic Therapy Duration in US Adults With Sinusitis. JAMA internal medicine. 2018;178(7):992-994. https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2674867
- Pouwels KB, Hopkins S, Llewelyn MJ, Walker AS, McNulty CA, Robotham JV. Duration of antibiotic treatment for common infections in English primary care: cross sectional analysis and comparison with guidelines. BMJ (Clinical research ed). 2019;364:l440. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6391655/
- Chastre J, Wolff M, Fagon JY, et al. Comparison of 8 vs 15 days of antibiotic therapy for ventilator-associated pneumonia in adults: a randomized trial. Jama. 2003;290(19):2588-2598. https://pubmed.ncbi.nlm.nih.gov/14625336/
- Singh N, Rogers P, Atwood CW, Wagener MM, Yu VL. Short-course empiric antibiotic therapy for patients with pulmonary infiltrates in the intensive care unit. A proposed solution for indiscriminate antibiotic prescription. American journal of respiratory and critical care medicine. 2000;162(2 Pt 1):505-511. https://pubmed.ncbi.nlm.nih.gov/10934078/
- Ryu S, Klein EY, Chun BC. Temporal association between antibiotic use and resistance in Klebsiella pneumoniae at a tertiary care hospital. Antimicrobial Resistance & Infection Control. 2018;7(1):83. https://pubmed.ncbi.nlm.nih.gov/30026941/
- Davies J, Davies D. Origins and evolution of antibiotic resistance. Microbiology and molecular biology reviews : MMBR. 2010;74(3):417-433. https://www.frontiersin.org/articles/10.3389/fmicb.2012.00018/full
- Aslam B, Wang W, Arshad MI, et al. Antibiotic resistance: a rundown of a global crisis. Infection and drug resistance. 2018;11:1645-1658. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6188119/
- National Center for Immunization and Respiratory Diseases DoBD. Active Bacterial Core surveillance (ABCs). CDC. https://www.cdc.gov/abcs/reports-findings/surv-reports.html. Published 2020. Accessed2020. https://www.cdc.gov/abcs/reports-findings/surv-reports.html
- CDC. Antibiotic Resistance Threats in the United States, 2019. Atlanta, GA. 2019. https://www.cdc.gov/drugresistance/pdf/threats-report/2019-ar-threats-report-508.pdf
- Bartlett JG, Gilbert DN, Spellberg B. Seven Ways to Preserve the Miracle of Antibiotics. Clinical Infectious Diseases. 2013;56(10):1445-1450. https://doi.org/10.1093/cid/cit070
- Gould IM, Bal AM. New antibiotic agents in the pipeline and how they can help overcome microbial resistance. Virulence. 2013;4(2):185-191. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3654619/
- Camponeschi G, Fast J, Gauval M, et al. An overview of the antiretroviral market. Current Opinion in HIV and AIDS. 2013;8(6). https://journals.lww.com/co-hivandaids/Fulltext/2013/11000/An_overview_of_the_antiretroviral_market.4.aspx
- Gohil K. Huge growth seen in hepatitis C market. P & T : a peer-reviewed journal for formulary management. 2014;39(7):517. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4103579/
- de Bruyn G, Saleh J, Workman D, et al. Defining the optimal formulation and schedule of a candidate toxoid vaccine against Clostridium difficile infection: A randomized Phase 2 clinical trial. Vaccine. 2016;34(19):2170-2178. https://www.sciencedirect.com/science/article/pii/S0264410X1600339X
- Varshney AK, Kuzmicheva GA, Lin J, et al. A natural human monoclonal antibody targeting Staphylococcus Protein A protects against Staphylococcus aureus bacteremia. PloS one. 2018;13(1):e0190537. https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0190537
- DÃez-MartÃnez R, De Paz HD, GarcÃa-Fernández E, et al. A novel chimeric phage lysin with high in vitro and in vivo bactericidal activity against Streptococcus pneumoniae. Journal of Antimicrobial Chemotherapy. 2015;70(6):1763-1773. https://academic.oup.com/jac/article/70/6/1763/729872
- Ghosh C, Sarkar P, Issa R, Haldar J. Alternatives to Conventional Antibiotics in the Era of Antimicrobial Resistance. Trends in microbiology. 2019;27(4):323-338. https://pubmed.ncbi.nlm.nih.gov/30683453/
- Huttner B, Saam M, Moja L, et al. How to improve antibiotic awareness campaigns: findings of a WHO global survey. 2019;4(3):e001239. https://gh.bmj.com/content/bmjgh/4/3/e001239.full.pdf
References for Commentary
- Talbot GH, Jezek A, Murray BE, Jones RN, Ebright RH, Nau GJ, Rodvold KA, Newland JG, Boucher HW; Infectious Diseases Society of America. The Infectious Diseases Society of America’s 10 × ’20 Initiative (10 New Systemic Antibacterial Agents US Food and Drug Administration Approved by 2020): Is 20 × ’20 a Possibility? Clin Infect Dis. 2019 Jun 18;69(1):1-11. doi: 10.1093/cid/ciz089. PMID: 30715222. https://academic.oup.com/cid/article/69/1/1/5305275
- Sato T, Yamawaki K. Cefiderocol: Discovery, Chemistry, and In Vivo Profiles of a Novel Siderophore Cephalosporin. Clin Infect Dis. 2019 Nov 13;69(Suppl 7):S538-S543. doi: 10.1093/cid/ciz826. PMID: 31724047; PMCID: PMC6853759. https://academic.oup.com/cid/article/69/Supplement_7/S538/5624004
- Zhanel GG, Golden AR, Zelenitsky S, Wiebe K, Lawrence CK, Adam HJ, Idowu T, Domalaon R, Schweizer F, Zhanel MA, Lagacé-Wiens PRS, Walkty AJ, Noreddin A, Lynch Iii JP, Karlowsky JA. Cefiderocol: A Siderophore Cephalosporin with Activity Against Carbapenem-Resistant and Multidrug-Resistant Gram-Negative Bacilli. Drugs. 2019 Feb;79(3):271-289. doi: 10.1007/s40265-019-1055-2. PMID: 30712199. https://link.springer.com/article/10.1007/s40265-019-1055-2
- Chahine EB, Sucher AJ. Lefamulin: The First Systemic Pleuromutilin Antibiotic. Ann Pharmacother. 2020 Dec;54(12):1203-1214. doi: 10.1177/1060028020932521. Epub 2020 Jun 4. PMID: 32493034. https://journals.sagepub.com/doi/10.1177/1060028020932521