Vivian Hayashi MD and Robert Smith MD, Mystery Quiz Section Editors
The patient is a 61 year old man presenting with one month of worsening shortness of breath. The patient has a history of alcoholism and was diagnosed with atrial fibrillation during a hospital admission for detox three years earlier. Warfarin …

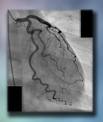
 By David Ecker, MD
By David Ecker, MD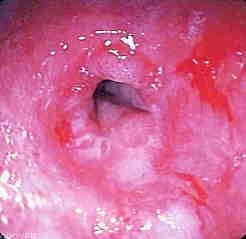 By Ramya Srinivasan, MD
By Ramya Srinivasan, MD By Maura RZ Madou, MD
By Maura RZ Madou, MD