 By Rhodes Hambrick
By Rhodes Hambrick
Peer Reviewed
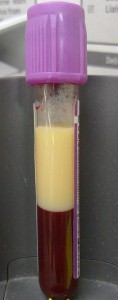
The atherosclerotic cardiovascular disease (ASCVD) risk associated with hyperlipidemia (HLD), readily apparent from the Framingham Heart Study1 of the mid-20th century, has been the target of innumerable attempted pharmacologic interventions …

 By Jonathan Glatt
By Jonathan Glatt By Elissa Driggin
By Elissa Driggin By James Barger
By James Barger By Tyler Litton, MD
By Tyler Litton, MD By Matthew B. McNeill, MD
By Matthew B. McNeill, MD By David Valentine, MD
By David Valentine, MD By David Pineles, MD
By David Pineles, MD